Venlafaxine is a commonly prescribed second-generation
antidepressant. It is well-known to psychiatrists because it is a second line
medication if SSRIs fail and for many psychiatrists it is another first-line
antidepressant. In some head-to-head comparisons with SSRIs venlafaxine has a
more favorable side effect profile. It does have the risk of discontinuation
symptoms and typical antidepressant side effects. I have noticed that the dose
escalation with venlafaxine seems to be out of proportion with SSRIs, bupropion,
and third-generation antidepressants.
Consider the following venlafaxine related scenarios:
1. A colleague comes into my office late in the day and
asks me: “Have you ever heard of venlafaxine causing sedation at higher doses?”
The patient in question was just increased from 187.5 mg to 225 mg - the
suggested max dose according to the FDA approved package insert.
2. I am asked to consult on patient who had extensive
pharmacogenomic testing in a different facility where she was told that she may
need to take 350 to 450 mg of venlafaxine per day based on that genetic
profile. She wants to make sure that she gets an adequate dose of the
antidepressant and is currently on 225 mg.
I reviewed the limitations of that approach with the patient and
potential side effects and I let her know that the commonest side effect I see
in people taking high-dose venlafaxine is excessive sedation or low energy in
the daytime. As we start to follow the recommended dose increase she discloses
that she has had sedation even at the 225 mg level. We decreased the dose to
150 mg and that side effect is gone. Her
depression is also gone.
3. I see a significant number of patients taking more than
300 mg per day of venlafaxine from the same geographic location in the United
States. They all tell me that the target dose in that location is 350 mg per
day and they are all experiencing numerous side effects. Many had dose
escalations into that range in a week or two - much faster than any increase I
have done.
What is wrong with this picture? Why are there a significant
number of people taking more than the recommended dose of venlafaxine in some
cases much more and appearing to have side effects? The roots of this prescribing behavior can be traced back to
old-school psychopharmacology. Proponents of that approach suggests that there
may always be a group of outliers that need to take higher-than-expected doses
of medications - typically antidepressants but there has also been a history of
excessive dosing of antipsychotic medications. People were generally more
cautious with more toxic medications like tricyclic antidepressants, monoamine
oxidase inhibitors, lithium, and various addictive compounds. They also seem to
be more cautious with SSRI type medications at least initially. It took over a
decade for me to see a dose of sertraline in excess of the maximum recommended
dose. While it is true that there are always outliers in terms of dose-response what is the best way to approach that problem.
I have attended medical education
courses where the lecturer suggested titrating the medication to the point of
toxicity and then reducing it back down to the next lowest dose. That
particular lecture was focused on treating anxiety disorders with SSRIs. I don’t
think that is the best approach. The best approach to me is one where the
patient recovers from anxiety or depression and the process does not experience
a single side effect. I know that can be done because I have been doing it for
decades.
That also brings me to what I think is a good research article that looks at optimal dosage ranges. It is a very large
meta-analysis of fixed dose randomized clinical trials that utilize the
specific antidepressants - citalopram, escitalopram, fluoxetine, paroxetine,
sertraline, venlafaxine, and mirtazapine.
The trials were identified by searching the literature and looking for
unpublished studies specifically by searching national drug licensing agencies
and requests directly to pharmaceutical manufacturers. Outcomes were noted at
eight weeks of treatment and defined as a 50% reduction on an observer rated
scale for depression. Dose equivalence
among medications was determined from previous studies and the recommendations
of the manufacturer. The article is written by researchers that I consider to be world experts in meta-analyses and the analysis of large data sets in psychiatry.
77 studies were identified from a total of 24,524 published
references and 4030 unpublished records.
27 were published, 21 or unpublished, and 29 were both published and
unpublished. The study showed too hard when treatment groups across all of the
medications of interest between the years 1986 and 2013.
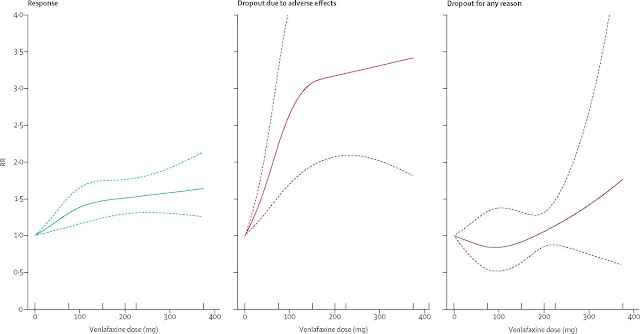
The authors calculated dose response, dropouts due to adverse effects, and dropouts for any reason. Relative risks (RRs) were calculated for
specific doses. The dose outcome relationships for venlafaxine are included in
the figures below from the original article.
The Response figure shows the significant increase of up to about 150 mg
and then a much more modest increase beyond that. The Dropout figure shows a
similar increase up to the 150 mg range. The Dropout for any reason was less
remarkable. The authors calculated that the 75-150 mg dose of venlafaxine was equivalent to 20
to 40 mg of fluoxetine (click to enlarge graphic)
The authors conclude that optimal acceptability of SSRIs
and venlafaxine and and mirtazapine occurs within the lower end of the licensed
dose range. They reconcile this with serotonin transporter (SERT) studies that
show that 80% SERT occupancy occurs at the minimum doses of SSRIs or
venlafaxine with further dose increases showing small increase in SERT
occupancy.
In the case of venlafaxine they suggest that noradrenalin
reuptake transporter (NET) may require higher doses of venlafaxine in the 225
mg to 375 mg per day range. Given the lack of efficacy of atomoxetine, a logical
question might be whether NET blockade adds much to the antidepressant effect.
The authors review other dose-efficacy studies of
antidepressants and point out that they are variable. The variability ranges
from optimal doses of fluoxetine in the 21-40 mg per day range to doses at the
recommended lower end of the range being superior. Response to doses in the
higher range were variable in some studies. One study found a significant
greater response for high-dose antidepressants but the dose of 40-50 mg
fluoxetine equivalents showed the greatest efficacy.
The authors considered strengths and limitations their
study. They thought that their state-of-the-art meta-analysis was a strength as
well as the size of the data set. They also examined dose dependency for both
efficacy and tolerability and acceptability. The limitations they
discussed included patient selection and dosing not reflecting clinical practice. They
also discussed the calculation of dose equivalency among antidepressants and
how that might be problematic.
Another obvious strength of this study is the calculation
of relative risks for response across SSRIs, venlafaxine, and mirtazapine. The
figures are modest but favor antidepressants across all dosage ranges with the
exception of mirtazapine at the 60 mg dose.
The authors don’t seem to mention it but it would seem that the optimal
dosage ranges could be predicted from the regulatory information since that is
based on dose ranging studies and tolerability studies. In that regard, the
conclusion about dose ranges don’t seem to be that surprising but they may be
needed given what is happening clinically.
Getting back to the issue with venlafaxine I see people
respond to dosing within the lower and of the range from 37.5 to 75 mg in many
cases. That same response rate continues up to the 150 mg dose and then starts
to diminish between two or 25 and 375 mg. Over that same range there is a
significant increase in dropout rates due to adverse effects.
How clinicians approach this new information will be
interesting. There will still be people like me and the conservative camp
looking for the first signs of side effects and toxicity and deciding at that
point whether to stop dose escalation. I explicitly tell people that the goal
is not to experience any side effects and that I doubt that people “get used to”
side effects. There are clearly clinicians out there who are
doing exactly the opposite and that is increasing the dose of venlafaxine and
advising people to either tolerate the side effects or expect that they will go
away.
The balance between therapeutic effect and side effects is
a central issue in all branches of medicine. In many cases, the severity of
adverse effects like an allergic reaction determines the decision. In the case
of the medication like venlafaxine making that decision can be complex. Some of
the side effects like sedation and lethargy at high doses can mimic symptoms of
depression. At this point in time neither pharmacogenomics or most plasma level determinations guarantees either tolerability or
efficacy.
Detailed analysis of the situation by an expert with a bias toward preventing side effects is required as the first step in any dose increase.
Detailed analysis of the situation by an expert with a bias toward preventing side effects is required as the first step in any dose increase.
George Dawson, MD, DFAPA
References:
1: Furukawa TA, Cipriani A, Cowen PJ, Leucht S, Egger M, Salanti G. Optimal dose of selective serotonin reuptake inhibitors, venlafaxine, and mirtazapine in major depression: a systematic review and dose-response meta-analysis. Published:June 06, 2019DOI: https://doi.org/10.1016/S2215-0366(19)30217-2.
Attribution:
Above figure of the venlafaxine dose response and drop outs are directly from the paper in reference 1 and used per the Creative Commons Attribution 4.0 International Public License.