Tuesday, September 27, 2016
The Reality Of Burprenorphine Therapy
It is increasingly popular for politicians and healthcare businesses to discuss their ideas about how to end the opioid epidemic that they started. One of the common themes is widespread availability of both buprenorphine maintenance therapy and naloxone opioid antagonist therapy for acute overdoses. I am certainly not opposed to either and in fact work in an addiction treatment environment where these are two of several medication assisted therapies used to treat addictive disorders. I am skeptical of the idea that broad prescribing of these therapies in either primary care clinics or some treatment settings will ever occur. Naloxone will be more readily available because there is a movement to create easy access without a prescription. That will never happen with buprenorphine. Last week - an article in JAMA backs up my skepticism (1).
The JAMA article looks at 3234 buprenorphine prescribers in the 7 states with the most buprenorphine prescribers. In their introduction the authors talk about the policy initiatives to increase the maximum patients per prescriber from 30 to 100 patients after a year. The average monthly patient census per month varied from 7 - 22 patients and a median monthly patient census of 13 patients. The duration of treatment episode was 53 days. This illustrates that the monthly census was well below the allowed limits and the duration of treatment was well below the recommended maintenance guideline of 12 months. They cite evidence that novice prescribers wanted more access to substance use counselors or other prescribers with more experience as potential limiting factors.
The authors of this article do not offer other explanations for the low rate of buprenorphine prescribing. I have a few. I really do not like stigma arguments. To me stigma seems like an excuse for not being able to overcome societal biases toward a particular problem. I don't see how you can train to be a physician and not have most of these biases wrung out of you. With addictions and mental illnesses there may be a stronger bias based on personal experience. Some physicians may have come from a family where the the father was an alcoholic or a heroin addict living homeless on the street and everybody was used to that idea. Some physicians may have come from families where the father was still drinking and dying of cirrhosis and the familiy opinion was that he "has a right to drink himself to death" rather than get treatment that he did not want in order to stop drinking. Other physicians may have come from families where father and his father both had severe alcoholism. Grandfather drank himself to death by the time he was 50. Father got treatment for his alcohol problem and was in stable recovery for years. All of these personal experiences and the reactions to them will affect how a physician approaches alcoholism and addiction.
Those biases are all part the the inevitable decision-making process that leads physicians down specific career paths. I have lost count of the number of times that another specialist told me that they really liked psychiatry and were considering the residency except for certain features of the field. A couple of examples include needing to try to predict suicide and aggression and live with the consequences or dealing with a certain diagnostic group like patients with severe personality disorders. People are less specific about addictions, probably because as medical students and interns we all see the severe effects. Most of the acute care hospitals where physicians train have 30-50% of their admissions based on the acute effects of alcohol or drug use. That includes many admissions for acute hepatitis, hepatic encephalopathy from cirrhosis, acute alcohol poisoning, acute overdoses on addictive drugs, and various psychiatric morbidities like delirium and psychosis from the acute effects of addictive drugs. It is less obvious but addictive drugs and alcohol are also overrepresented as reasons for admission to surgical trauma units and burn units. Most interns and residents see these effects first hand and develop both short term and long term perspectives on these problems.
This seems like another case of managers and politicians not appreciating the intense interpersonal aspects of medicine. Physicians are all not foot soldiers just waiting for the next assignment from a policy maker. Physicians have probably carefully selected the type of practice they want to be in and there are more than the technical aspects of the speciality that were considered. It takes a unique skill set to treat people with addictions. Treating and maintaining an opioid addict in treatment long enough with buprenorphine maintenance for them to realize any benefit is a very unique skill. Being affiliated with other buprenorphine prescribers is also a necessity to provide cross coverage for patients. Speciality care centers for addiction seem like an idea to me that does not get a lot of consideration. Trying to run a buprenorphine maintenance program in a practice environment that is rationed to the degree it currently is does not seem feasible to me. Adding buprenorphine maintenance as just another task for a busy primary care physician practicing primary care medicine is not likely to work. It should be obvious that these physicians have more than enough to do right now.
There is a lot more to it than increasing the maximum numbers of opioid addicted patients on buprenorphine maintenance and trying to treat as many people as possible. The data from this paper illustrates that. There is also the issue of the preventing the pool of opioid users from increasing while trying to treat those who are currently dependent on these drugs. That seems like the best long term option to me.
Addressing this complicated problem takes more than a licensed buprenorphine prescribing physician sitting behind a desk who is willing to prescribe it. It takes better infrastructure including managers who are enlightened enough to get that physician the kind of resources they need to do the work. I never hear politicians or policymakers talking about that.
George Dawson, MD, DFAPA
Reference:
1: Stein BD, Sorbero M, Dick AW, Pacula RL, Burns RM, Gordon AJ. Physician Capacity to Treat Opioid Use Disorder With Buprenorphine-Assisted Treatment. JAMA. 2016 Sep 20;316(11):1211-1212. doi: 10.1001/jama.2016.10542. PubMed PMID: 27654608.
Saturday, September 24, 2016
An Excursion into the Psychiatric News - Blurred Lines Between Business and Professional Organizations
 |
| Psychiatry Eclipsed |
Before anyone says that this is me going off the rails again - consider one small factor. For over 30 years I have been paying the American Psychiatric Association (APA) significant amounts of money in annual dues. Last year it was about $935. During some of those years, I thought it might be useful to also donate to their political action committee and I gave them significantly more money. All the time, I was expecting something to reverse the inexorable deterioration in the practice environment and the rationing of mental health services. During that time, I witnessed first hand the deterioration of psychiatric services in the state of Minnesota to the point that there is now a mandate that county sheriffs have priority in admitting their mentally ill prisoners to state psychiatric hospitals. The psychiatrists in the state have no say in who gets admitted to these facilities or the severely rationed number of inpatient beds in the state. The reason for professional organizations as I understand them is to speak for and advance the profession, support its members and advocate policies that benefit the people that interact with the profession. In the case of psychiatry that is the patients that we treat, their families, and the larger society. All I have to do is pick up a copy of the Psychiatric News to doubt that these mandates are very relevant anymore.
I will say in advance that in my assessment the APA does a fair job in terms of education and professionalism. I have criticized them in this area in the past for not keeping the treatment guidelines up to date and relevant. Subsequent to that there was a new guideline published. Access to the educational materials is not contained in the membership dues. A subscription to Psychiatry Online or the CME Journal Focus are additional charges as are CME credits for reading articles in the American Journal of Psychiatry. There is also a CD version of courses and presentations at the APA Annual Meeting that is available for a significant cost. The educational and professional materials are definitely available and some of them are first rate - but they do come at a price.
My biggest problem with the APA has been the total lack of rigor in countering the deterioration of the practice environment and in many cases seeming to directly participate in initiatives that are counter to the interests of psychiatrists and their patients. Thumbing through the September 16, 2016 edition of the Psychiatric News provides some ready examples.
On page 1, there is a story Everett Appointed head of New SAMHSA Office. The story is all about APA President Elect Anita Everett, MD assuming a new position as chief medical officer at SAMHSA - the lead federal agency for mental health and substance use treatment. A direct quote from Dr. Everett: "Having a psychiatrist as a member of the leadership team at SAMHSA will enable psychiatrists to join other mental health and public health professionals in guiding the federal component of the nation's behavioral health systems." My emphasis on behavioral health. As far as I am concerned SAMHSA is a pro-managed care government bureaucracy - like most of them. Secondly, there are plenty of psychiatrists out there who have been chief medical officers for managed care companies and I would challenge anyone to tell me why they are necessary and what they have accomplished. Managed care companies tell psychiatrists what to do. They are not interested in a reasonable practice environment, reasonable inpatient settings of even professional standards. They are interested in cheap, rationed care by overworked clinicians. I don't doubt Dr. Everett's qualifications or good intentions. I don't think I am going out on a limb too far to say that she is going to be severely restricted by the current bureaucracy with a strong managed care bias. That is not good for psychiatrists and it certainly is not good for patients.
The other story on page 1 seems worse - Are Psychiatrists prepared for Health Care Reform? Yes and No. I really can't think of a more nauseating term in the medical literature than health care reform. I have been hearing those hot little words for the entire length of my career. I heard them from the Clintons back in the days when Hillary Clinton headed up the health care reform efforts during the first Clinton presidency. Some students of the topic like to recall that for one reason or another the initiative worked on by Hillary Clinton was not successful. I think that depends on the standard. There certainly was no expected global program, but it did make managed care a household word and set managed care as the predominant bias in all further discussions of health care reform. Like most history - people seem to have forgotten this and the Clinton administration (and all that followed) as having a strong managed care bias. The article suggests that psychiatrists need to get on board with the collaborative care model - another managed care rationing technique. In the span of 3 decades psychiatry has gone from protesting managed care rationing (especially because it affects us and our patients the most) to suggesting you really have to get on board with this. The usual buzzwords like further workforce development and merit-based payment reforms are evident. When professional standards are abandoned what is merit-based payment reform? In all likelihood it has to do with rationing techniques rather than quality medical care. Paragraph after paragraph in this article read like a managed care playbook. Maybe the only way to see through all of this pro management rhetoric is to have actually worked in one of these systems of care. Try working in one with a manager who is reimbursed to extract the maximum amount of productivity while not providing resources to physicians in the system. In that case I believe the management buzz word is creativity. In a rationed environment there is often an audacious statement about creativity as a solution rather than additional personnel. Most reasonable people would be shocked at what constitutes merit-based payment or the hold back procedures before you can get to that level. Just another in a long line of meaningless cliches flowing from health care reform.
As you might imagine I was a little tense and clammy as I went on to page 2. There I was an editorial piece by APA President Maria A. Oquendo, MD. It was title Why 'Physician Heal Thyself' Does Not Work. I was mildly optimistic that she might come to the same conclusion that I have about physician burnout - it is not a disease it is just bad management. Dr. Oquendo began with a description of the recent suicides of a psychiatric resident and a medical student. She presents the epidemiology of physician suicide and suicidal ideation. She points out for example that suicide is the second leading cause of death for physicians between the ages of 24 and 35. She discusses the stigma of a psychiatric diagnosis and the gap between problems and who gets treated. Her solution is self identification of depression and excessive alcohol use. There seem to be other factors that are operative. She quotes a six fold jump in PHQ-9 scores during internship - using that as a metric for depression. I can't help but think how physicians and trainees are more isolated now than ever. No matter what the setting we had great teams when I was an intern and resident. We took care of one another and we had attending physicians who cared. I addressed some of that in my previous burnout article. Nobody discusses what it is like to train in a managed care and rationed environment today compared with medical care as usual in the past. During my last stint in a hospital I did not see well developed teams anywhere. Most of the senior physicians who did a lot of the teaching and tended to view themselves as affiliated with residents had been replaced by hospitalists. Entire teaching services had been replaced. Non-medical management has left many medical institutions very arid places with few personnel and limited collegiality. That is exactly the wrong environment for depressed and stressed physicians. Training programs everywhere can help residents by making sure they build collegiality and that team factor in all of their rotations. They need to provide highly motivated faculty who have the interests of trainees in mind as a priority. The teams I am referring to here are teams of physicians, not teams that contain administrative staff telling physicians what to do.
The article most directly related to managed care hegemony was "Medical Necessity in Psychiatry: Whose Definition Is It Anyway? by Daniel Knoepflmacher, MD. The title is of course purely rhetorical. Like many things in medicine today medical necessity has nothing to do with medicine. It is a pure business definition designed to give the appearance of legitimacy to what is a pure business driven decision. The decisions are made by people with no appreciation of human biology or its complexity. They are people who seem to think that a lot of meaningless business metrics somehow apply to the practice of medicine. At the worst (and most probable) they are simply rationing to make a profit. I would call them nerds but I really don't think that they are that smart.
In the article, Dr. Knoepflmacher makes that point. There is not even a standard business definition of medical necessity. Companies can basically say and do whatever they want. He traces the history of the term and how various groups define it today. Interestingly one of the largest managed care companies states that it is for payment purposes only. He points out the overemphasis on acute or crisis care rather than professional guidelines or standards. I would argue that in psychiatry, managed care companies do a very poor job of addressing acute care by using only a dangerousness metric. The term cost effectiveness is incorporated into some of the definitions in the 1960s. The acclaimed Mental Health Parity and Addiction Equity Act of 2008 lacks any definition of medical necessity or a more useful definition of medical appropriateness. That may explain why this legislation has had negligible impact. Dr. Knoepflmacher's thesis can be best summarized in the sentence:
"Without universal medical necessity criteria for mental health care, clinicians and their patients are saddled with a concept highly susceptible to abuse by insurers."
I would take it a step further. The abuse has been institutionalized at this point. Clinicians find themselves abused at every fork in the road. Any time a psychiatrist refills a medication for a colleague or because the treatment setting has changed they are subjected to abusive prior authorization processes that are in place purely to harass physicians into giving up and patients to the point that they are paying out of pocket instead of using the insurance they have paid for. In that case Congress is directly responsible for erecting two multibillion dollar industries and inserting them between the physician and their patient. I would also propose a much better limit than arbitrary medical necessity criteria. It should be apparent that any managed care company can get around legislation and rules that they lobbied to pass. I propose that physicians recommend a course of treatment to patients and that they are totally removed from the payment process. No more wasting time with insurance company employee-reviewers. No more conflict of interest in favor of big business. The physician recommends treatment. The insurance company tells the patient if they will pay for it. Other than civil action by the patient, the only oversight should be a panel of physicians carefully screened for conflict of interest at the state level to mediate disputes (sorry no insurance industry insiders).
Highlighting these four articles creates a portrait of what is wrong with the APA. Like other professional organizations it has clearly bought into the pro-management zeitgeist that is generally sold by American businesses and government. The general idea is that there are business managers that know more about what you do and can tell you what to do - irrespective of your professional training and experience. That idea is a mile wide and an inch deep. Anyone with middle school analytic skills should have come to the same conclusion as Dr. Knoepflmacher - about 20 years ago. His article is there now as a necessary reminder that there is a much better way to do things. Instead of affiliating with these outrageous business practices - they should be actively resisted at every level. That should include the practice and training environments. There is nothing worse for physicians and patients than wringing the humanity out of medical practice.
And there is nobody better at doing that than current healthcare business managers.
George Dawson, MD, DFAPA
Attributions: The graphic is all me. It is supposed to represent a progressive overlap by government and business interests with the profession. There are psychiatrists that work in the overlap areas and some who work just in the black and gray zones. The field is still plodding along as though it is an autonomous profession.
Sunday, September 18, 2016
Is Melatonin A Benign Supplement?
Before I get too carried away the answer to the question is most likely yes - it is a benign supplement. That is based on all of the studies and reviews I have about melatonin used to treat insomnia and other sleep disorders. Nobody seems to report any major side effect from even very high doses taken for periods of time. Those same reviews have a lot of qualifiers. As an example some will say that doses in the 4-6 mg per night range are unlikely to cause major side effects. Others will suggest that even though melatonin use is widespread, there have not been any large clinical trials to assess long term safety. There probably never will be. When people ask me about the safety of melatonin that is exactly what I tell them. Individual use of over-the-counter melatonin varies greatly. The average self-administered dose that I encounter these days is 10 milligrams. The range of outliers is to the high side. Nobody uses the 1 mg or 3 mg tablets but there are people using 10-20 mg.
My concerns come from a number of perspectives. First there is the issue of normal excretion of melatonin and pharmacokinetics. Second there is the role of melatonin in other systems in the body. And third there is the question of the toxicology of melatonin. In the case of supplements, the presumed toxicology is often based on the exposure of large numbers of people to the supplement and no alarming or immediate side effects. Melatonin is ubiquitous in some tissues in the body and this gives the impression that it may be a benign compound. On the other hand it is a metabolite of 5-HT (serotonin) and this has additional implications. 5-HT is a highly politicised molecule with unquestionable roles in human physiology and pharmacology.
When I start to think about the general approach to this problem - the first thing I look at is what the physiological levels of melatonin might be in both blood and CSF. The published medical literature is scant. Normal levels are often determined as part of an experimental intervention like peripheral sympathectomy. In one study (1), the normal diurnal fluctuations were noted with a peak ranges of peak plasma levels varied from 122-660 pmol/L, and the peak CSF levels from 94-355 pmol/L. In this study the authors demonstrated that bilateral T1-T2 ganglionectomy abolished both the diurnal rhythms and resulted in lower levels of melatonin suggesting that the peripheral sympathetic nervous system has input into melatonin secretion.
Other studies have looked at the effects of melatonin supplementation on plasma and CSF levels. This is always important because average natural melatonin secretion in humans is about 0.15 mg per day. As I previously indicated supplementation is many times that. An early study (2) showed that oral melatonin supplementation led to rapid increases in blood and CSF melatonin. The authors also compared the ratio of CFS/blood melatonin and noted it was constant before and after supplementation suggesting that blood is the source of CSF melatonin. Recent studies (4-6) suggest that melatonin is secreted directly into the third ventricle from the pineal recess or that there may be central or peripheral compartments of melatonin for different effects.
There was a recent comprehensive review of the pharmacokinetics of melatonin. The authors reviewed 22 high quality studies looking at oral or IV dose ranges of 0.1 mg to 100 mg. Cmax (maximum plasma concentration following the dose) ranged from 72.1 (10 ml/h; 0.02 mg, IV) to 101,163 pg/ml (100 mg, oral). Tmax (time to peak plasma concentration) ranged between 15 (2 mg) and 210 min (10 mg). T1/2 (half-life) ranged from 28 (0.005 mg, IV) to 126 min (4 mg, oral). The response to melatonin for insomnia is unpredictable and no dose response curve has been determined. Of course there are a wide range of available melatonin preparations from pharmacies and health food stores. Even in the research, it is often difficult to say what preparation was used, but the bioavailability is quoted as 15%.
The sleep research on melatonin shows that (as most clinician know) it has weak sleep effects but variability does exist. Most people will notice very little effect. Some will claim that they were "knocked out" and strongly sedated even the next day - an effect that is hard to reconcile with the short half-life. The lack of a dose-response curve makes it difficult to determine dosing but a review in an authoritative sleep text (8) says that most studies use a dose of 4-6 mg and that the timing of the dose (1-3 hours before sleep) may be an important factor. I have been advised myself by a sleep expert that a 1 mg dose of melatonin 3 hours before sleep may be optimal because it entrains the circadian rhythm of that individual and have seen that work in many cases. The weak effects on sleep EEG to me suggest a strong placebo component.
Getting back to the side effect issue - I was surprised to find a few pages on melatonin in last week's New England Journal of Medicine in their Clinical Implications of Basic Science Research section (9). These authors discuss the implications of the MTNR1B variant as a risk factor for Type 2 diabetes mellitus. This variant leads to an overexpression of MT2 melatonin receptors on pancreatic beta cells. Melatonin in this case leads to a G-protein-coupled receptor (GPCR) initiated cascade that inhibits insulin secretion. They reviewed the epidemiology of diabetes and the facts that Type 2 diabetes is typically a combination of insulin resistance in muscle and fat cells, increased hepatic glucose output and no compensatory insulin release. They reference an experiment where the daily melatonin (4 mg dose) for 3 months reduced first phase glucose induced insulin secretion in an oral glucose tolerance test compared with baseline before melatonin secretion. They point out that there has been some epidemiological work that associates shift work with susceptibility to diabetes mellitus. They conclude that typical doses of melatonin of 4 mg/day or less are not likely to be associated with decreased insulin release and talk about the application of melatonin in jet lag with dosing for a few days. They also point out in the 3-month long study that overall glucose tolerance was hardly affected and baseline glucose levels returned after 2 hours of dosing. That may not be as assuring to psychiatrists who are seeing their patients take 5-10 mg indefinitely along with other medications that may cause metabolic syndrome.
To me this is also further evidence of just how crude many of our clinical trials are that look at the issue of metabolic syndrome and diabetes in clinical populations. Whenever I discuss consent for atypical antipsychotics and the metabolic issues, I always tell people that weight gain and increased appetite is common. I also tell them that I have seen people develop diabetes from these medications who were rail thin and never gained an ounce. The 150 risk alleles for Type 2 diabetes mellitus, the thousands of associated intracellular signalling proteins, and the 300 GPCRs expressed in pancreatic beta cells probably has something to do with that.
Biological complexity rarely leads to simple answers.
I will probably encourage a lot of insomniacs from taking melatonin when there has been no clear benefit. I will probably also discourage the practice of taking high dose (> 5 mg) of melatonin for the same reason.
George Dawson, MD, DFAPA
References:
1: Bruce J, Tamarkin L, Riedel C, Markey S, Oldfield E. Sequential cerebrospinal fluid and plasma sampling in humans: 24-hour melatonin measurements in normal subjects and after peripheral sympathectomy. J Clin Endocrinol Metab. 1991 Apr;72(4):819-23. PubMed PMID: 2005207.
5: Leston J, Harthé C, Brun J, Mottolese C, Mertens P, Sindou M, Claustrat B. Melatonin is released in the third ventricle in humans. A study in movement disorders. Neurosci Lett. 2010 Jan 29;469(3):294-7. doi: 10.1016/j.neulet.2009.12.008. Epub 2009 Dec 11. PubMed PMID: 20004701.
6: Skinner DC, Malpaux B. High melatonin concentrations in third ventricular cerebrospinal fluid are not due to Galen vein blood recirculating through the choroid plexus. Endocrinology. 1999 Oct;140(10):4399-405. PubMed PMID: 10499491.
7: Harpsøe NG, Andersen LP, Gögenur I, Rosenberg J. Clinical pharmacokinetics of
melatonin: a systematic review. Eur J Clin Pharmacol. 2015 Aug;71(8):901-9. doi: 10.1007/s00228-015-1873-4. Epub 2015 May 27. Review. PubMed PMID: 26008214.
8: Krystal AD. Pharmacological Treatment: Other Medications. in Kryger MH, Roth T, Dement WH. Principles and Practice of Sleep Medicine, 5th Edition. Elsevier Saunders, St. Louis, 2011. p. 916-930.
9: Persaud SJ, Jones PM. A Wake-up Call for Type 2 Diabetes? N Engl J Med. 2016 Sep 15;375(11):1090-2. doi: 10.1056/NEJMcibr1607950. PubMed PMID: 27626524. (to full text link).
Attribution:
Serotonin metabolism graphic is from VisiScience.
melatonin: a systematic review. Eur J Clin Pharmacol. 2015 Aug;71(8):901-9. doi: 10.1007/s00228-015-1873-4. Epub 2015 May 27. Review. PubMed PMID: 26008214.
8: Krystal AD. Pharmacological Treatment: Other Medications. in Kryger MH, Roth T, Dement WH. Principles and Practice of Sleep Medicine, 5th Edition. Elsevier Saunders, St. Louis, 2011. p. 916-930.
9: Persaud SJ, Jones PM. A Wake-up Call for Type 2 Diabetes? N Engl J Med. 2016 Sep 15;375(11):1090-2. doi: 10.1056/NEJMcibr1607950. PubMed PMID: 27626524. (to full text link).
Attribution:
Serotonin metabolism graphic is from VisiScience.
Thursday, September 15, 2016
Hospitalists.....
I was a hospitalist before the word was fashionable. It was July 1988 and I had just completed a 3 year post residency stint at a community mental health center as part of a public health service scholarship payback. For one of those years I commuted another 300 miles to keep a community hospital psychiatric unit open. I headed for the hospital where I did my rotating internship in Internal Medicine, Pediatrics and Neurology. It was the only real metropolitan inpatient treatment setting I had known at that point. In my residency program, the interns were split up into two groups and each group worked at one of the major county hospitals in the Twin Cities. It was a unique setting at that time because psychiatrists provided almost all of the medical coverage. They had to be able to diagnose and treat a lot of common medical problems, write for all of the patient's medications, attend to acute medical problems and do the appropriate diagnosis and triage. I had a wide range of medical problems admitted directly to me ranging from gunshot wounds to delirium. Any psychiatrist working in these conditions realizes that the term "medically stable" is a relative one. I had many patients admitted to my service with severe medical problems only because they also had a severe psychiatric disorder and were symptomatic at the time. In many cases I had to rapidly assess them and transfer to medicine or an intensive care setting.
I had excellent back up by consultants and many of them to this day are some of the best physicians I have ever seen. But they really did not want to hear from me unless I had a very specific probable diagnosis and most of the evaluation was done. There are not too many places in psychiatry where jobs like that exist anymore. If anyone asks me about similar positions - I actively discourage them from accepting a similar job. With this arrangement the work is far too long and all of the medical care is provided for free - psychiatrists do not get any extra credit for it.
In those days there were six of us covering 3- 20 bed wards, five days a week. The ads for psychiatrists these days often speak of "psychiatric hospitalists" - but every one of them specified no medical coverage. They also tend to leave out the part that it is basically a rapid triage and discharge position and the job is to either maintain or cooperate with high discharge rates. The only thing they have in common with the Internists and Family Physicians who have come to be designated as hospitalists is that they work 7 days on and 7 days off. A schedule that very few people question.
I naturally picked up this week's copy of the New England Journal of Medicine to see what the two perspective pieces on hospitalists (1,2) had to say. I was also interested because my brother is an Internist and over the years we have discussed the issue at length. The initial essay by Wachter and Goldman documents the rapid rise of hospitalist care as a medical specialty. Since 2003 the number of hospitalists has increased 5-fold to 50,000. That makes hospitalists the largest speciality within Internal Medicine. They cite the growth of managed care, Medicare DRG payments, and possible evidence as reasons for the growth of the field. I am always skeptical of the term efficiency especially when it is combined with the term quality. I guess it is difficult for some people to accept the fact that managed care and Medicare DRG payments are rationing mechanisms that are tied to quality only by the tenuous thread of government and healthcare company rhetoric and advertising. The other critical question is efficiency for who? It certainly is more efficient to administer a group of physicians who work 7 days on and 7 days off and happen to all be in the same chain of command. It is a lot easier to get them to accept the role of rationing care in the interest of the hospital or health care group than the patient's personal physician who may see their part of their role as patient advocacy.
The authors have an interesting take on the deficiencies of the model. They talk about the 7- days-on, 7-day-off model as implying that during the off period the physician is literally off and suggests that time might be better spent contributing to key institutional programs. To me - this schedule seems more conducive to burnout and anyone who works it needs the off time to fully recover. I have never seen a study on the cognitive efficiency during the 7-days-on, but my conversations with hospitalists suggests that by day 6 it starts to plummet. With hospitalists supplanting specialists and subspecialists as inpatient attendings they suggest that trainees have less exposure to basic and translational science. Although not stated in the article, the model involves eliminating whole blocks of specialty care. I worked at a hospital where an entire Neurology service was eliminated by hospitalist care. When I questioned that decision I was told: "We have an Internist who is interested in strokes." Changing neurologists from attendings to consultants with hospitalists as the primary physicians for neurological problems changes the entire nature of care. It also changes the associated nursing care when staff have no ongoing interest in the care of complex neurology patients. The authors also note that hospitalists do not seem to have focused on investigating common inpatient illnesses. They suggest possible remedies - but these seem like major problems that will only get worse with the increasing business rather than academic emphasis in medicine.
Gunderman points out that as opposed to the usual delineators of speciality care - patient age, physician skillset and body system hospitalists are delineated only by patient location. He doesn't make it explicit but what is the relationship between location and his list of putative benefits? Looking at length of stay for example - that could logically follow as a concentrated effort in the location, but is that a clinical effort or an administrative one? He points out that the increasing number of hospitalists per se, cannot be taken as evidence of benefit and that perverse incentives exist. I agree with the most perverse being the low reimbursement incentive for high volume practice. Seeing complex inpatients with a high frequency of initial and discharge assessments may reduce the volume necessary for productivity demands. When I was a psychiatric hospitalist, this dimension was manipulated in a number of ways. I was initially told, I was responsible for a set number of inpatient beds. At some point there was a great deal of pressure for me to start running outpatient clinics because they would be more "interesting" than just seeing inpatients. I resisted that and had significant leverage because nobody else wanted to do my job. I eventually did run a Geriatric Psychiatry and Memory Disorder Clinic for many years while continuing inpatient work. That clinic was eventually closed by administrators because they claimed our productivity was not high enough to work with a nurse. The neurologist and I needed all of the collateral data that she collected to do our work. The expectation was that we would see complex dementia patients and do everything that the nurse in our clinic did - so we closed. In over two decades of political wrangling around inpatient productivity the current consensus is that covering 10-12 inpatient beds is a reasonable approach. At one point I was covering 20 beds with the help of an excellent physician assistant but at the cost of doing no teaching.
The critical aspect of Gunderman's thesis is his emphasis on the physician-patient relationship exemplified by this sentence:
"The true core of good medicine is not an institution but a relationship - a relationship between two human beings."
He points out that physicians being affiliated with institutions creates significant conflicts of interest, isolates hospital staff from the rest of the medical community and that naturally leads to less expertise in the entire community. It also creates the illusion that an institution rather than the relationship is the core of medical care and it is not. Government-business constructs like Accountable Care Organizations have a similar effect. I have experienced this first hand many times as I dealt with the iterations of hospitalists consulting on my patients. In one case I talked with a young hospitalist about a patient with Type 2 diabetes mellitus. The patient had a trace of renal insufficiency and was on metformin - a medication that is risky in that context. The hospitalist advised me to call the primary care Internist taking care of the patient because "He has been doing it a long time and probably knows more about it than I do." In addition to the relationship - there is clear expertise associated with caring for people with multiple complex medical problems for years in an outpatient setting - compared to a few days as an inpatient. The medical industrial complex does not adequately value that expertise.
I think that there is room for hospitalists and psychiatric hospitalists. They have to be focused on the needs of both the patient and the patient's outpatient physician. There have to be clear goals for the hospitalization and one of those goals is what the patient's personal physician would like to see accomplished. Since making the transition to strictly outpatient care - it is clear that the hospitalists no matter who they might be don't have much control over who gets admitted to the hospital and what happens there. They are having less to say about when a person is discharged. This is probably more true for psychiatry than medicine and it results in a large number of psychiatric outpatients not being able to access needed care.
And I can't help but notice that inpatient hospital medicine is still a far better resource than inpatient hospital psychiatry.
George Dawson, MD, DFAPA
References:
1: Wachter RM, Goldman L. Zero to 50,000 - The 20th Anniversary of the Hospitalist. N Engl J Med. 2016 Aug 10. [Epub ahead of print] PubMed PMID:27508924.
Sunday, September 11, 2016
Minnesota's Suicide Prevention Plan
I have pointed out several times on this blog that a number of non-medical forces in the state of Minnesota have been successful in making a mediocre mental health system into one that is on the brink of becoming a travesty. My curiosity was naturally piqued when I heard that we now had a suicide prevention plan released just in time for Suicide Prevention Week and Suicide Prevention Awareness month. How is suicide prevention and awareness possible in a seriously deteriorating nonsystem of care? Who are the people writing this report and what does it say? As a person actively involved in suicide prevention every day of my career - I decided to read it and give my impressions here. The full text is available to anyone off the Minnesota Department of Health web site.
Scanning the document, it is very readable. The main body is about 23 pages long with relatively large font and much if it is organized more like an outline rather than a document. For reasons I will outline below - it could have been a lot briefer. Task Force member are listed and it appears that none of them are psychiatrists. Of the 19 listed Task Force members - one of them is a physician. The stated goal of the work is:
"To reduce suicide in Minnesota by 10% in five years, 20% in ten years, ultimately working towards zero ....." (page 7)
That is certainly a laudable goal. There are recent reviews and ongoing debates about whether suicide can be eliminated and a recent consensus statement says no (1). Buried on page 19 is the statement "Encourage health care systems to implement the Zero Suicide Model. There is a link provided to SAMHSA on this model and it is the product of non-experts. Because of its promotion of managed care I do not consider SAMHSA to be a reliable source of information or expertise. A review of what is available the Zero Suicide Model (4) illustrates that it is basically a management heavy model of what used to be considered standard psychiatric care before psychiatric care was disrupted by business interests with the usual EHR kowtowing.
As far as reduced rates or total suicides in the state a useful question is whether or not the trends in suicide rates or total number of suicides is a real trend in Minnesota or it reflects expected variation. The second important question is whether it is a population wide phenomenon or it reflects subpopulations that are impacting on the statewide rates. The authors attempt to answer these questions by showing an increase in the rates of suicide from 8.9 per 100,000 (n=440) in 2000 to 12.2 per 100,000 (n=683) in 2013 - the last year of complete data for the report. The ratio of men:women who died by suicide was 4:1. The rate across the US was 12.6 - the Minnesota rate is slightly less than the national rate. Among subgroups of the population the American Indian group had the highest rate at 17.2 per 100,000 (n=70) followed by White at 12 per 100,000 (n=2,941). Black or African Americans had the lowest rate at 6.9 per 100,000 (n=104). American Indian Youth (10-24) had the highest rate at 28.0 per 100,000 (n=30).
A standard method to determine if death trends related to risk factors or illness are significant is joinpoint regression analysis developed by the National Cancer Institute to analyze trends in cancer deaths. Since then it has been used by both the CDC and researchers (3) looking at trends in suicide rates. I did not see the application of this kind of analysis to the rates over the 14 year period of time discussed in the article. That does not mean it was not done, just not apparent. At the minimum an analysis of longer term trends should be accomplished along with comparisons to other macro indicators like economic variables would be interesting as a basis for preventive recommendations.
The authors leap into their model called a social ecological model of suicide that was adapted from the World Health Organization. A graphic is included in the statement. The model appears to be generally applied - it has been widely adopted by the WHO and the CDC as a way to address suicide and violence but also colon cancer and a host of other medical problems. It seems to be a modern equivalent of the old nature versus nurture or schizophrenigenic mother argument. Cataloguing all of the perceived deficiencies in the environment is not the same thing as discovering the mechanism or cause of a specific problem in a specific person. Obvious examples abound. The vast majority of people who have had significant childhood adversity in the environment do not attempt or commit suicide. That is a relevant question because a better approach may be studying those people and trying to figure out how they survived and either adapt to chronic levels of insomnia, anxiety, and depression or resolve it. A consciousness based model may be the best approach. The authors here seem to say that all of these social and economical factors need to be addressed and that is the approach that they are going to use to reduce the suicide rate. Even using that approach they overstep the limits of the model and end up using a familiar political approach.
The political approach that I am referring to is to assume that somehow they know more about suicide than the professional trained to address it. I speak only for psychiatrists, but this is a serious overstepping of authority. I was board certified in Psychiatry in 1988 and it was well known at the time that if a candidate did not demonstrate that they could interview a person and assess their potential for suicide and aggression that they would fail the oral examination. Psychiatrists have been focused on timely assessments of suicide and aggression for decades and it is incorporated into treatment guidelines at every level. Those assessments are done very day by practically every psychiatrist working that day. And yet the Minnesota Plan has the following guidance:
4. Train professionals and community/cultural leaders to increase awareness of suicide and prevention efforts and mental health and wellbeing. (p.15)
3. Train professionals and community/spiritual/cultural leaders to better understand how to talk to and encourage those at risk to access help. (p. 16)
The authors here can make these statements because they are as non-specific as possible. Psychiatrists are not mentioned at all in the document. Neither are other mental health professionals. Speaking only for psychiatrists again, we are practicing psychiatry with people who have the most severe forms of mental illness because we can assess and treat suicide and aggressive behavior. We are certainly not looking to any state agency for training or accountability. We are accountable to the people we treat and professional standards. Furthermore we are acutely aware of the deficiencies in care in this state and input from psychiatrists would probably have been useful. The tactic of pretending to tell professionals how to do their job and generally behave has been used by the managed care industry for years. It is disappointing but not unexpected to see in in a document from a state who has been so friendly to that industry.
1. Public education on suicide - especially the statistics the risk factors, and the fact that suicide is a treatable and resolvable condition.
2. Means reduction - at a public health level these are some of the most successful interventions. As an example, people need to know that just having a firearm in the home is the single most risk factor for suicide. I get a letter every year telling me that I have to report the number of abortions that I performed last year and all of the abortion complications in Minnesota. These same people have access to all of my professional information and know that I have never performed an abortion. I have never investigated the origin of this letter but can only conclude it is a law written by an anti-abortion legislators hoping to shame physicians into not performing legal abortions. Why isn't anyone using a more functional approach and sending conceal-carry permit holders a letter on suicide and gun possession. Why isn't it being taught in public health classes in the schools? Why doesn't everyone know that most deaths by firearms in this country are from suicide?
3. Cultural permissiveness toward substance use - Minnesota has medical cannabis laws and an active group of recreational cannabis promoters. There is a current nation wide movement to view psychedelics and hallucinogens as medications and psychotherapeutic agents. There is very little discussion of the downside. We are also in the midst of a highly lethal opioid epidemic. As an addiction psychiatrist many of the people I talk with get to the point in their addiction that in their search for getting high - they don't care if they live or die. They knew they were taking lethal or near lethal amounts and did not care. In other cases, certain people with alcohol use problems will become suicidal only if they are intoxicated. These correlates of substance use disorders and the suicidal lethality of substance use is practically unknown to most people. It is not trendy or cool to push back against overwhelming pressure to get high - but that is exactly what needs to happen. Stay sober and you reduce the chances of ever being suicidal.
4. Don't depend on managed care companies to provide a reasonable system of care - The record is in and it is not a good one. The idea that managers whoever they might be are going to teach or coerce professionals into providing better care for people with suicidal thinking when they have been working for three decades to do just the opposite seems absurd to me. If the government wanted to do anything, it would be to provide functional oversight of these companies and their ongoing rationing of care. Every state should have a physician review agency for treatments that is outside of the usual same company reviewers and insurance industry insiders placed on state regulatory boards. That board should have the last word in what treatments are necessary. Community mental health centers need to be refunded to provide adequate levels of care and they cannot be un like managed care companies.
These are a few of my thoughts today. I might add another couple of bullet points as they come to mind. This is a serious topic that deserves additional discussion and one I have been thinking about most of the time with varying levels of intensity for 30 years.
George Dawson, MD, DFAPA
References:
1: Shain B; COMMITTEE ON ADOLESCENCE. Suicide and Suicide Attempts in Adolescents. Pediatrics. 2016 Jul;138(1). pii: e20161420. doi: 10.1542/peds.2016-1420. PubMed PMID: 27354459.
That is certainly a laudable goal. There are recent reviews and ongoing debates about whether suicide can be eliminated and a recent consensus statement says no (1). Buried on page 19 is the statement "Encourage health care systems to implement the Zero Suicide Model. There is a link provided to SAMHSA on this model and it is the product of non-experts. Because of its promotion of managed care I do not consider SAMHSA to be a reliable source of information or expertise. A review of what is available the Zero Suicide Model (4) illustrates that it is basically a management heavy model of what used to be considered standard psychiatric care before psychiatric care was disrupted by business interests with the usual EHR kowtowing.
As far as reduced rates or total suicides in the state a useful question is whether or not the trends in suicide rates or total number of suicides is a real trend in Minnesota or it reflects expected variation. The second important question is whether it is a population wide phenomenon or it reflects subpopulations that are impacting on the statewide rates. The authors attempt to answer these questions by showing an increase in the rates of suicide from 8.9 per 100,000 (n=440) in 2000 to 12.2 per 100,000 (n=683) in 2013 - the last year of complete data for the report. The ratio of men:women who died by suicide was 4:1. The rate across the US was 12.6 - the Minnesota rate is slightly less than the national rate. Among subgroups of the population the American Indian group had the highest rate at 17.2 per 100,000 (n=70) followed by White at 12 per 100,000 (n=2,941). Black or African Americans had the lowest rate at 6.9 per 100,000 (n=104). American Indian Youth (10-24) had the highest rate at 28.0 per 100,000 (n=30).
A standard method to determine if death trends related to risk factors or illness are significant is joinpoint regression analysis developed by the National Cancer Institute to analyze trends in cancer deaths. Since then it has been used by both the CDC and researchers (3) looking at trends in suicide rates. I did not see the application of this kind of analysis to the rates over the 14 year period of time discussed in the article. That does not mean it was not done, just not apparent. At the minimum an analysis of longer term trends should be accomplished along with comparisons to other macro indicators like economic variables would be interesting as a basis for preventive recommendations.
The authors leap into their model called a social ecological model of suicide that was adapted from the World Health Organization. A graphic is included in the statement. The model appears to be generally applied - it has been widely adopted by the WHO and the CDC as a way to address suicide and violence but also colon cancer and a host of other medical problems. It seems to be a modern equivalent of the old nature versus nurture or schizophrenigenic mother argument. Cataloguing all of the perceived deficiencies in the environment is not the same thing as discovering the mechanism or cause of a specific problem in a specific person. Obvious examples abound. The vast majority of people who have had significant childhood adversity in the environment do not attempt or commit suicide. That is a relevant question because a better approach may be studying those people and trying to figure out how they survived and either adapt to chronic levels of insomnia, anxiety, and depression or resolve it. A consciousness based model may be the best approach. The authors here seem to say that all of these social and economical factors need to be addressed and that is the approach that they are going to use to reduce the suicide rate. Even using that approach they overstep the limits of the model and end up using a familiar political approach.
The political approach that I am referring to is to assume that somehow they know more about suicide than the professional trained to address it. I speak only for psychiatrists, but this is a serious overstepping of authority. I was board certified in Psychiatry in 1988 and it was well known at the time that if a candidate did not demonstrate that they could interview a person and assess their potential for suicide and aggression that they would fail the oral examination. Psychiatrists have been focused on timely assessments of suicide and aggression for decades and it is incorporated into treatment guidelines at every level. Those assessments are done very day by practically every psychiatrist working that day. And yet the Minnesota Plan has the following guidance:
4. Train professionals and community/cultural leaders to increase awareness of suicide and prevention efforts and mental health and wellbeing. (p.15)
3. Train professionals and community/spiritual/cultural leaders to better understand how to talk to and encourage those at risk to access help. (p. 16)
Objective 2.2 Expect providers who interact with individuals at risk for suicide to routinely assess for access to lethal means. (p. 17)
The authors here can make these statements because they are as non-specific as possible. Psychiatrists are not mentioned at all in the document. Neither are other mental health professionals. Speaking only for psychiatrists again, we are practicing psychiatry with people who have the most severe forms of mental illness because we can assess and treat suicide and aggressive behavior. We are certainly not looking to any state agency for training or accountability. We are accountable to the people we treat and professional standards. Furthermore we are acutely aware of the deficiencies in care in this state and input from psychiatrists would probably have been useful. The tactic of pretending to tell professionals how to do their job and generally behave has been used by the managed care industry for years. It is disappointing but not unexpected to see in in a document from a state who has been so friendly to that industry.
I can say without a doubt that most Minnesotans seeking acute care for a family member with suicidal thinking or suicidal behavior will be disappointed. The severe rationing of psychiatric services has resulted in a lack of resources that would be comparable to any other medical emergency. Families are frequently directed to hospital emergency departments where mental disorders are viewed creating congestion and inconvenience. The social workers making the assessments there know that placement options are extremely limited. The legislative response to their own rationing of psychiatric services has been to mandate that the patient be transferred to the nearest bed and that can be hundreds of miles away. Once hospitalized most people realize the the inpatient units that were supposed to help them are grim and unsanitary places where they main goal is to convince the psychiatrist that they are no longer suicidal so that they can be discharged home. The family may find themselves in the uneasy position of monitoring their suicidal family member at home while they are trying to get them adequate treatment. It is the logical progression of events to a government and insurance industry standard that dangerousness is the only reason a person can be admitted to a psychiatric unit these days. Managed care reviewers call the physicians and nurses in charge looking for that day when the patient doesn't use the word suicidal. At that point according to the insurance industry - the patient must be discharged. They always have the excuse that it is up the the attending psychiatrist - but that has become a modern day joke. The psychiatrist's own administration will insist that the patient be discharged or he/she might need to find another job.
How should it work? Crisis care for suicidal or aggressive people should be based on an informed approach to the problem. Risk factors (and protective factor) analysis is really an insufficient approach. The approach that suicide is an epiphenomenon of other psychiatric disorders is also a limited approach. There are certainly correlates of high suicide rates in most major psychiatric disorders - but how that person came to consider suicide is generally a unique pathway even in the case of most extreme mental illness. First, emergency department triage must go. The only reason it exists is that there is inadequate funding for community mental health centers and their own crisis services. The paradigm for this model is Dane County Mental Health Center in Madison, Wisconsin. This has been one of the epicenters of community psychiatry in the US. They have an active crisis service that runs all day long until 11PM. They a have a walk in crisis center. They are adequately staffed to avoid long waits and they do active crisis psychotherapy. Second, inpatient psychiatry needs serious revision. We can no longer accept the idea that a person in crisis sits on an inpatient unit until they say they are no longer suicidal. Granted there are always social interventions along the way but a lot more needs to happen. The units need to be clean, calm and comfortable places. They need to provide an array of active services to treat both severe problems and address suicidal thinking. They need to keep longitudinal data on the efficacy of their interventions. They need to provide assessments and treatments for alcohol and substance use disorders. There are many people who become suicidal only under the influence of alcohol or street drugs. Most importantly, they need to admit people with severe problems even if they are not saying that they are suicidal at the time. The reasons for that are twofold. The majority of people with significant mental illnesses are not being treated. If they cannot function this is a logical point to provide treatment and reduce the transition to suicide risk. The other reason is that there are many severely ill people who clearly cannot function with their current level of distress. They may have attempted suicide in the past. Their psychiatrist knows they are high risk in the community, but currently there are no hospital or residential settings where these people can be admitted.
Read the document and make your own assessment. The goals of modifying the social fabric in various communities in Minnesota seem unrealistic to me. I think that this group and the parent document is overreaching - not just in the scope of what can be done for apparently very little funding but also the gross inconsistencies in government and business. There are no bigger conflicts of interest these days than a government that seems to want to advertise that they are solving your problems when they are doing just the opposite and businesses that do the same. A functional state department of health should use the usual public health tools with education being at the top. Some more attainable and straightforward goals would be:
Read the document and make your own assessment. The goals of modifying the social fabric in various communities in Minnesota seem unrealistic to me. I think that this group and the parent document is overreaching - not just in the scope of what can be done for apparently very little funding but also the gross inconsistencies in government and business. There are no bigger conflicts of interest these days than a government that seems to want to advertise that they are solving your problems when they are doing just the opposite and businesses that do the same. A functional state department of health should use the usual public health tools with education being at the top. Some more attainable and straightforward goals would be:
1. Public education on suicide - especially the statistics the risk factors, and the fact that suicide is a treatable and resolvable condition.
2. Means reduction - at a public health level these are some of the most successful interventions. As an example, people need to know that just having a firearm in the home is the single most risk factor for suicide. I get a letter every year telling me that I have to report the number of abortions that I performed last year and all of the abortion complications in Minnesota. These same people have access to all of my professional information and know that I have never performed an abortion. I have never investigated the origin of this letter but can only conclude it is a law written by an anti-abortion legislators hoping to shame physicians into not performing legal abortions. Why isn't anyone using a more functional approach and sending conceal-carry permit holders a letter on suicide and gun possession. Why isn't it being taught in public health classes in the schools? Why doesn't everyone know that most deaths by firearms in this country are from suicide?
3. Cultural permissiveness toward substance use - Minnesota has medical cannabis laws and an active group of recreational cannabis promoters. There is a current nation wide movement to view psychedelics and hallucinogens as medications and psychotherapeutic agents. There is very little discussion of the downside. We are also in the midst of a highly lethal opioid epidemic. As an addiction psychiatrist many of the people I talk with get to the point in their addiction that in their search for getting high - they don't care if they live or die. They knew they were taking lethal or near lethal amounts and did not care. In other cases, certain people with alcohol use problems will become suicidal only if they are intoxicated. These correlates of substance use disorders and the suicidal lethality of substance use is practically unknown to most people. It is not trendy or cool to push back against overwhelming pressure to get high - but that is exactly what needs to happen. Stay sober and you reduce the chances of ever being suicidal.
4. Don't depend on managed care companies to provide a reasonable system of care - The record is in and it is not a good one. The idea that managers whoever they might be are going to teach or coerce professionals into providing better care for people with suicidal thinking when they have been working for three decades to do just the opposite seems absurd to me. If the government wanted to do anything, it would be to provide functional oversight of these companies and their ongoing rationing of care. Every state should have a physician review agency for treatments that is outside of the usual same company reviewers and insurance industry insiders placed on state regulatory boards. That board should have the last word in what treatments are necessary. Community mental health centers need to be refunded to provide adequate levels of care and they cannot be un like managed care companies.
These are a few of my thoughts today. I might add another couple of bullet points as they come to mind. This is a serious topic that deserves additional discussion and one I have been thinking about most of the time with varying levels of intensity for 30 years.
George Dawson, MD, DFAPA
References:
1: Shain B; COMMITTEE ON ADOLESCENCE. Suicide and Suicide Attempts in Adolescents. Pediatrics. 2016 Jul;138(1). pii: e20161420. doi: 10.1542/peds.2016-1420. PubMed PMID: 27354459.
3: Puzo Q, Qin P, Mehlum L. Long-term trends of suicide by choice of method in Norway: a joinpoint regression analysis of data from 1969 to 2012. BMC Public Health. 2016 Mar 11;16:255. doi: 10.1186/s12889-016-2919-y. PubMed PMID:26968155.
4: Hogan MF, Grumet JG. Suicide Prevention: An Emerging Priority For Health Care.Health Aff (Millwood). 2016 Jun 1;35(6):1084-90. doi: 10.1377/hlthaff.2015.1672. PubMed PMID: 27269026.
Disclaimer:
I had no input into the Minnesota Suicide Prevention Plan and I know none of its authors. I accessed it online and read it.
I had no input into the Minnesota Suicide Prevention Plan and I know none of its authors. I accessed it online and read it.
Monday, September 5, 2016
Why Is The Cirrhotogenic Dose Of Alcohol Important?
 |
The Standard Drink http://rethinkingdrinking.niaaa.nih.gov/How-much-is-too-much/What-counts-as-a-drink/Whats-A-Standard-Drink.aspx
|
One of my main tasks during an interview is assessing the medical condition of the patient. That is important in determining associated comorbidity, potential causes of psychiatric symptoms, factors that might affect how any medications I assess or prescribe are metabolized, medical tests that I need to order and follow, the insight and functional capacity of the patient - are they aware of the physical problem and doing something about it, and any referrals that I need to suggest and make to primary care physicians or specialists. When I see people who are using significant amounts of alcohol - alcoholic liver disease and cirrhosis are high on that list. In many cases they are seeing me and already have a diagnosis of cirrhosis, but nobody else in the current system of care seems to know that. Continuity of care is really not an administrative priority in American health care. We all practice in administrative silos defined by electronic health records (EHRs) that don't talk to one another and produce very low quality printouts. Just recently I reviewed an EHR printout that was 30 pages long. As usual the hospital and dates of service were not evident. About 20 of those pages was a consultant's report that pulled in every lab the person across their lifetime - spread in uneven columns across the pages.
How to get to these important but obscured diagnoses? It is always important to ask about hepatitis and cirrhosis. I also ask about infectious and alcoholic types. Some standard review of systems include questions about jaundice and that is a good one to ask. Non-standard question include asking about seeing a gastroenterologist or liver specialist. I will ask about specific imaging like hepatic ultrasounds, CTs, and MRIs. I will ask if there has ever been upper GI endoscopy or colonoscopy, the indications, and what they were told about the findings. I will ask about whether a doctor has ever told my patient to stop drinking and why? In the population of moderate to heavy drinkers that I see, it is rare to find all of a person's care provided at one location. There are typically emergency department visits and hospitalizations that the primary care MD is not aware of. There may be attempts to treat the alcohol use problem and there is often not a very strong medical component associated with that treatment. The patient may be actively avoiding contact with medical care out of fear of what might happen with the illness. All of these factors make it extremely important not to miss the diagnosis and at the minimum recommend optimal care for that person.
From a strictly historical standpoint, the key question is whether there are some historical markers that allow for the stratification of risk. Can you tell whether your patient might have cirrhosis just based on their drinking history? Moderate to heavy drinkers vary considerably in their veracity on reporting alcohol use. It may depend on the phase of treatment. A reliable description of consumption may occur early in treatment after a conscious decision to "come clean" about it. There will be a number of people who are not ready to stop drinking irrespective of the quantity they are drinking and the problems that it has caused. They might be in the assessment because of external factors like family members who are upset by their drinking. There are also the limits of memory. If a person acknowledges 20-30 years of moderate to heavy drinking and multiple DWIs in their early 20s - they are unlikely to provide a detailed description of their progression of drinking and may only hit a few of the high points - like when they started experiencing blackouts on a daily basis. In my experience, most moderate to heavy drinkers focus on the last 2 or 3 years of drinking. That can create the impression that they have not been drinking long enough to cause significant damage.
Part of the problem in taking the clinical history of drinking is that there can be a bewildering array of drinks and measures - often to the point that the clinician is not sure about absolute quantities or alcohol concentrations. The literature on cirrhosis and alcoholic liver disease often requires a conversion to standard drinks or grams. Those drink sizes especially the ones that are culturally determined (there are definitely drinking subcultures in the US) or self-determined can lead to wide variation in the amount of alcohol actually consumed. Collateral information is always very useful. From the graphic at the top of this page 1.5 fluid ounces of 80 proof (40%) alcohol or the equivalent in any one of those drinks is considered a standard drink in the US. That is 14 grams or 0.6 ounces of pure alcohol. The amounts that I hear about being consumed include a mini bottles (50 ml), a pint (473.2 ml), a fifth (750 ml), a liter (1000 ml), and a handle (1500 ml). Consuming the entire container of these beverages is the equivalent of taking 1, 10.7, 17, 22, and 33.8 - 1.5 ounce standard drinks respectively. In the literature the standard drink size in Australia is 10 grams of alcohol or 30 ml of 40% alcohol rather than the 14 grams specified in the US. That results in more drinks per beverage or container.
The National Institute on Alcohol Abuse and Alcoholism (NIAAA) has several definitions that are based on consumption that are useful. Binge drinking is defined as 5 or more drinks on a single occasion for men or 4 more more drinks on a single occasion for women - usually in less than 2 hours. Heavy drinking is defined as 15 or more drinks per week for men and 8 or more drinks per week for women. 9% of the US population exceeds both the single day and weekly consumption limits of these definitions. 28% of the US population will exceed either the single day limit or the weekly limit. 37% always drink within low-risk limits and 35% never drink. Those results are based on a sample of 44,000 Americans 18 years of age and older.
What are the estimates of alcohol use that cause cirrhosis? The first time I encountered this concept was in a Medical Clinics of North America reference (1) that suggested 15 pint years of drinking a pint of whiskey per day for 15 years. The American College of Gastroenterology makes a different estimate of 20-40 grams of alcohol daily - will result in liver damage in most women. They go on to specify that 80 grams of alcohol per day will lead to cirrhosis in men in 10 years and the same amount of daily alcohol consumption will lead to cirrhosis in women in 5 years. They also specify that in their use, 4 drinks is 4 - 5 ounces of distilled spirits so the standard drink size is less than the usual definitions. Converting all of those numbers into standard drinks -
20 grams = 1.4 standard drinks
40 grams = 2.9 standard drinks
80 grams = 5.7 standard drinks
In other words 5.7 standard drinks per day will result in cirrhosis in men in 10 years or cirrhosis in women in 5 years. On a clinical basis, I have seen very young people with alcoholic cirrhosis and the youngest were women in their late 20s. So the range for cirrhosis in the literature ranges from a low of about 1/2 pint of 80 proof alcohol per day for 5 or 10 years to 1 pint of 80 proof alcohol per day for 15 years.
The Australian National Health and Medical Research Council (NH&MRC) recommends that the maximum standard drinks per day for men is 4 and for women is 2. The range between the high and low estimates of toxicity is considerable given the fact that a pint of distilled spirits contains 10.7 standard drinks. The pint-a-day drinker exceeds both the NIAAA maximum recommended single day and weekly consumption.
There are a number of variables that affect the individual pharmacokinetics of alcohol and ultimate toxicity. Patterns of consumption are also important. Knowing the range of alcohol consumption that may have already impacted the patient is useful in terms of deciding if the history is accurate and how the treatment plan may need to be modified. It is also useful to know from a public health perspective, especially in the current era of liberalizing policies and attitudes about intoxicants.
George Dawson, MD, DFAPA
References:
1: Lefton HB, Rosa A, Cohen M. Diagnosis and epidemiology of cirrhosis. Med Clin North Am. 2009 Jul;93(4):787-99, vii. doi: 10.1016/j.mcna.2009.03.002. Review. PubMed PMID: 19577114.
Supplementary 1:
The dose of alcohol that is associated with pancreatitis is 4 or 5 drinks daily for a period of 5 or more years.
Forsmark CE, Vege SS, Wilcox CM. Acute Pancreatitis. N Engl J Med 2016; 375: 1972-1981.
Supplementary 2:
British National Health Service guidelines based on a standard drink of 25 ml of 40% alcohol.
Attribution:
Graphic at the top of this post is from the NIAAA we site Rethinking Drinking and is in the public domain at the references URL.
Wednesday, August 31, 2016
The Conscious Experience of Pain
 |
| Drawing of Pain Matrix from reference 2 with permission. |
One of the main problems with the assessment and treatment of chronic pain is that there are no quantitative or even good qualitative measures of whether pain exists and how much pain is really there. The current crisis of opioid overprescription began as an initiative to treat pain more aggressively and that started based on the use of a 10 point scale to estimate pain. There are many problems associated with that approach but the main one is that it is completely based on the patients self report. Self report is probably not the best measure when prescribing medications with a significant secondary gain component. Since that scale is used as a basis for potentially high risk therapies - better metrics would be very useful.
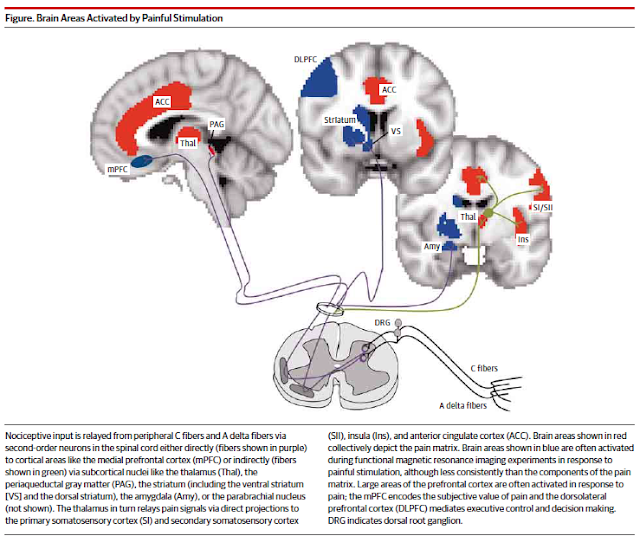
That brings me to two papers that I caught a little earlier this year in JAMA Neurology on the Pain Matrix. The first is a research letter on the pain matrix. The authors define the pain matrix as the set of brain structure that are activated by nociception or pain perception. As a general example they describe the general brain structures like the anterior cingulate cortex, thalamus, and insula. They cite evidence that these activated structures are considered a possible biomarker for drug discovery and legal proceedings. The paper is designed to test the veracity of this potential biomarker for pain. Their model was the administer mechanical noxious stimuli to subjects with congenital insensitivity to pain. These subjects had SCN9A mutations in the sodium channel of sensory neurons that results in loss of pain sensation but preservation of tactile sensation. For a discussion of the polymorphisms of this gene see reference 3 and the link on Congenital Insensitivity to Pain (CIP) (4). There were two pain free subjects and 4 controls. All subjects were scanned with a 3-T fMRI. They were also asked to rate the stimuli on two dimensions - sensation and pain using a 0 (no pain or sensation) to 10 (most intense pain or sensation).
The test subjects and control reported the same responses to sensation in terms of the subjective ratings with mean ratings(standard deviations) of 4.6(0.5) and 4.4(1.2) respectively. The painful stimulus was not rated as painful by the subjects but at a level of 3.2(1.8) by the controls. Most importantly there were no differences on fMRI scanning between the groups with similar levels of activation seen in the thalamus, anterior cingulate gyrus, insula, and pain matrix as a whole.
The fMRI results of the pain matrix response in normal controls and patients who are congenitally unable perceive are extremely interesting. Both groups had similar tactile sensation. The authors suggest that caution must be used when interpreting the imaging of this pain matrix for studies looking at the treatment of chronic pain. At another level, they seem like another addition to a long line of neuroimaging studies that do not seem to correlate very well with what they claim to represent. An accompanying editorial by Geha and Waxman discusses the fact that the pain matrix has been validated in hundreds of studies using different nociceptive input. They point out that some researchers equate activation of the pain matrix with the conscious perception of pain. They review some of the evidence against the pain matrix argument. One group has shown that activation of the pain matrix is multimodal. They show how context (monotonous versus novel stimuli) and multisensory and multimodal processing is important. These authors point out that they have shown fMRI activity in the pain matrix in chronic pain patients without any stimulus. There cite a study that looks at how the pain matrix is activated in the subacute stages of chronic pain (6-12 weeks) and then as it becomes chronic at up to one year it shifts to emotional circuitry in the medial prefrontal cortex. The authors also describe emotional and reward related decision making by the ventral striatum and medial prefrontal cortex, and how that activity decreases when chronic pain is successfully treated with carbamazepine while other areas of the pain matrix were unchanged. Plasticity is also cited as being important both at the clinical level with some basic science support showing that hippocampal neurogenesis was necessary to develop chronic pain behavior in rodents.
This research is extremely interesting at two levels. The first is a possible route to quantitative assessments of chronic pain. A lot of that will depend on a lot more data on the resting state of these brain systems and what changes can be consistently measured. Having lived through the era of quantitative EEGs - I see too many similarities here to not be skeptical. It is also not possible to do fMRI studies on chronic pain patients - there are just too many. Like most psychiatric disorders we need a rapid, inexpensive marker that our patient likely has chronic pain and a measure of severity would be useful. The second level is broadly important and that is figuring out how human consciousness occurs and how the individual conscious states of chronic pain patients differs.
Until then - I will be paying close attention to the arguments for and against the pain matrix and research papers that use this description.
George Dawson, MD, DFAPA
References:
1: Salomons TV, Iannetti GD, Liang M, Wood JN. The "Pain Matrix" in Pain-Free Individuals. JAMA Neurol 2016 Jun 1;73(6):755-6. doi: 10.1001/jamaneurol.2016.0653. PubMed PMID: 27111250.
2: Geha P, Waxman SG. Pain Perception: Multiple Matrices or One? JAMA Neurol 2016 Jun 1;73(6):628-30. doi: 10.1001/jamaneurol.2016.0757. PubMed PMID:
27111104.
3: Tang Z, Chen Z, Tang B, Jiang H. Primary erythromelalgia: a review. Orphanet Journal of Rare Diseases. 2015;10:127. doi:10.1186/s13023-015-0347-1.
3: Tang Z, Chen Z, Tang B, Jiang H. Primary erythromelalgia: a review. Orphanet Journal of Rare Diseases. 2015;10:127. doi:10.1186/s13023-015-0347-1.
4: Congenital Insensitivity To Pain (CIP). Genetics Home Reference. National Library of Medicine. Link.
Attributions:
1: From reference 2 above. The figure is used with permission of the American Medical Association from JAMA Neurology per the above reference. License Number 3897150095337; License Date:
Jun 26, 2016
Subscribe to:
Posts (Atom)



