Tuesday, June 9, 2015
Delirium Reinvented
One of my colleagues posted an article from the The Atlantic on delirium to her Facebook feed a few days ago. Most of my colleagues in that venue are hospital, consultation-liaison, addiction or geriatric psychiatrists and we diagnose a lot of delirium. Entitled the Overlooked Danger of Delirium in Hospitals it makes it seem like this is some kind of new and strange diagnostic category. The article talks about the prevalence, the association with critical illness and advanced age, and the diagnostic overlap of dementia and delirium. We hear from an Internal Medicine specialist Sharon Inouye, MD about the need to correctly diagnose and prevent delirium. She mentions that as opposed to a decade ago, physician and nurses are all taught about delirium. There is mention of the CAM (Confusion Assessment Method) that Inouye developed. Like all health care articles there are estimates of the massive cost of delirium as well some prevention techniques. There is also political concern that Medicare will declare delirium a "never" event with penalties for any hospital with cases of delirium. That would be unfortunate because it makes a mistake that also seems to be made in this article - that delirium is a manifestation of many illnesses, especially the kind of illnesses that patient's are hospitalized for.
The article seemed odd to me because it was written from the perspective that delirium is an iatrogenic preventable event! Certainly that can be the case. Delirium is a primary feature of hundreds of different disorders and recognizing delirium and those etiologies is potentially life saving. Delirium can mimic psychiatric conditions due to the presence of hallucinations and delusional thinking. For example, it is entirely possible to see a patient in the emergency department with apparent paranoid delusions and miss the fact that they happen to be delirious. Sometimes the only sign is that the patient is inattentive and when vital signs are checked they have an elevated temperature. This can be a common presentation of viral encephalitis in younger patients or urinary tract infections in the elderly. It is bad form to miss either of those diagnoses and attribute the symptoms to a psychiatric disorder. Another common form of delirium that is missed is drug or alcohol intoxication or withdrawal states. Some intoxicants will render the patient totally unable to care for themselves until they are detoxified. Other deliriums from alcohol or sedative withdrawal are life threatening and can be associated with seizures and other life-threatening states. An acute change in a person's mental state resulting in delirium needs to be recognized and assessed as a medical emergency.
One of the first cases of delirium that I ran into after residency was a case of cerebral edema that I was consulted on because of "hysterical behavior". After that, I worked in and eventually ran a Geriatric Psychiatry and Memory Disorders Clinic for about 8 years. The majority of people coming to that clinic had dementia of some sort. They would see me and a neurologist. We started out with an internist who was also a geriatric specialist, but that turned out to be overkill in terms of the number of medical specialists seeing each person in an outpatient clinic. We eventually opted for records from the patient's primary care physician. One of the most valuable functions of that clinic was our ability to follow people with prolonged deliriums. Once a delirium has been established by a disease state and that state has resolved the delirium can persist for months. Some of the outliers in that clinic took up to 6 months to clear. We found that in many cases, the patients were extensively tested for intellectual ability and functional capacity when they were in the delirious state and told that they had dementia. It was always instructive for the patient and family to get the testing repeated when we were sure the delirium had resolved and find that they had been restored to baseline. Many people know their full scale IQ score and were relieved to see that they were back to that level of functioning.
A valuable lesson from working in that clinic and in hospital settings was the use of the electroencephalogram (EEG) as a possible test for delirium. EEGs are commonly viewed as diagnostic tools to determine if a person is having seizures, but they also contain a lot of information about brain metabolism. EEGs can be difficult to interpret especially if the patient is on a number of medications that affects cerebral metabolism. There are two broad categories of EEG patterns for delirium: one with a predominance of slow frequencies (designated theta and delta) and one with faster frequencies (designated beta). We found a number of people with very significant cognitive impairment that was thought to be either a psychiatric disorder or a dementia but with a profound degree of slowing more consistent with a delirium.
Delirium is an augenblick diagnosis for most psychiatrists. The patient could appear disinterested, apathetic, agitated, or overtly confused. It occurs in situations where brain physiology is compromised such as post surgical/anaesthesia states, drug intoxication states, drug reaction states, or possible physical illness delirium should be high on the differential diagnosis. The Atlantic article makes it seem like knowledge about delirium is something very recent, but psychiatrists have been focused on it for a long time. In the first two iterations of the DSM, delirium was subsumed under the categories of acute and chronic brain syndromes (DSM-I 1952) and organic brain syndromes (DSM-II 1968). The current diagnostic code and name has been with us since the DSM III in 1980. One of the early experts in delirium was Zbigniew J. Lipowski, MD, FRCP(C) - a Professor of Psychiatry from the University of Toronto. His first text on the condition was Delirium: Acute Brain Failure in Man published in 1980. That was followed by his classic text, Delirium: Acute Confusional States published in 1990. A comparable text from a neurological standpoint was Arieff and Griggs Metabolic Brain Dysfunction in Systemic Disorders published in 1992.
Any psychiatrist trained in the past 30 years should be able to diagnose delirium and come up with a differential diagnosis and monitoring or treatment plan. A significant number of people can be followed on an outpatient basis as long as they are in a safe environment with the appropriate level of assistance. The main goal of treatment is to make sure that the primary medical illness that led to the problem has been treated. There are no known medications that will accelerate the resolution of these symptoms and medical management usually involves getting rid of medications that can lead to cognitive problems. That can include benzodiazepines, antidepressants and antipsychotics but also more common medications like antihistamines and anticholinergic medications that are used for various purposes. Like most psychiatric interventions in our health care system, clinics with staff interested in doing this work are few and far between generally because they are rationed resources.
There is a current movement underway to train Family Physicians and Internists (like Dr. Inouye) to recognize and prevent delirium. In the minority of hospitals where psychiatrists work they are also a clear resource. A delirium in a previously healthy person should signal a fairly comprehensive evaluation to figure out what happened.
And whenever there is a question of whether a person has a delirium or a psychiatric disorder - call a psychiatrist. Psychiatrists know a lot about delirium and have for decades.
George Dawson, MD, DFAPA
Reference:
Sandra G. Boodman. Overlooked Danger of Delirium in Hospitals. The Atlantic. June 7, 2015.
Supplementary 1: The graphic is a standard EEG. I tried to post a slowed EEG seen in delirium, but the publisher wanted what I consider to be an exorbitant fee for a non-commercial blog. If anyone has a slow anonymous EEG laying around, send me a copy and I will post it.
Sunday, June 7, 2015
The Myth of Monolithic Psychiatry
One of the familiar strategies of the various antipsychiatry factions out there is the monolithic psychiatry tactic. A monolith can be a monument that is often a large rectangular block of stone. The most recognizable monolith in my time was the recurring black monolith in 2001 - A Space Odyssey. A monolith can also refer to "a large and impersonal political, corporate, or social structure regarded as intractably indivisible and uniform." In that sense, a monolith can just be a fact. I could refer to just about every government agency and insurance company that I have to deal with as monolithic. They couldn't care less about anything that I say to them or how infuriating it is that I have to deal with them. Their only interest is in their corporation and doing the absolute minimum that might cost them something and they are very good at it. In practical terms that means authorizing any treatment I am forced to ask them about. But in a new twist many of these organizations also aggressively trying to make any physicians they are working with - look bad. They must think there is some advantage in keeping physicians on the defensive.
The beauty of monoliths is that no matter how hard you try there is no way to break in and get what you want. No matter how many times I call the government bureaucracy in charge of dealing with managed care company complaints, I will get the same predictable runaround. The first several lengthy calls will result in me talking to people who are not even sure that they should be talking with me. They will send me to somebody in another building in an obscure department and eventually the calls will stop again. I have wasted many hours of my life trying to crack into this monolithic state government bureaucracy without success. I think it also illustrates some additional defining characteristics of monoliths - secrecy, anonymity, and a lack of accountability. Eventually you end up talking with people so far removed from the problem, it is not clear how you ended up in touch with them in the first place. Their names and positions are meaningless. It is clear that they can't help you and if you wanted to complain about them it would not make any difference. They are so far removed from your original problem it doesn't matter anymore. You can rage against the monolith as much as you want and it doesn't make any difference. There may be a conspiracy of monoliths if you are working with an employer who wants you to try to cooperate with them and makes that part of your contract. Employers like that are often monoliths themselves, with various strategic firewalls around the organization to prevent employees from providing feedback on company policy. Monoliths often trigger conspiracy theories because they are either intentional or unintentional conspiracies.
That brings me to the interesting phenomenon of monolithic psychiatry. Assume for a moment that all psychiatrists in the country are in a monolithic structure like the one I described for the state bureaucracy. It might make sense for someone to rage against the monolith by declaring psychiatry is heavily influenced by the pharmaceutical industry or psychiatry overprescribes medications or psychiatry isn't interested in psychotherapy or whatever anyone wants to apply to the monolith. Since we are talking about a monolith, whatever applies to one psychiatrist applies to them all which logically makes the criticism one big absurdist editorial.
There are many things wrong with that picture. Psychiatrists have the most diverse population of any medical specialty and it is the farthest to the left. More psychiatrists are liberals and psychiatry is the only specialty group that is predominantly composed of Democrats. The broad range of interests of psychiatrists are evident at any American Psychiatric Association (APA) meeting and various annual subspecialty meetings. Courses are available on a broad range of medical, neuroscientific, and psychosocial topics. Psychiatrists work in a number of specialty areas and it is very likely that certain practices are highly specialized and focus only on the diagnosis and treatment of specific conditions. That is not the structure of a monolith. The total number of psychiatrists varies on the source. The American Medical Association (AMA) census in 2010 put the number at 42,885. The Census put the number at 40,600 in 2009 and of those 26,200 were office based. According to the Bureau of Labor Statistics there are only about 25,000 psychiatrists who are employees of organizations. The remainder are in private practice. The American Psychiatric Association sent me the following data on the membership for the past 15 years.
As a measure of monolithic behavior, in one of the most critical APA election in recent years regarding maintenance of certification (MOC) only 6,943 members voted. Action requires a vote of at least 40% of the membership. Interestingly the MOC vote occurred in 2011, the year of the lowest number of members. The total vote was not close to the 40% number, but it exceeded the vote for the President Elect and Secretary by about 1,300 votes each. Presidents are typically elected by less than 20% of the members. These facts illustrate that the majority of psychiatrists in this country at any one time are being directly influenced by employers and in the overwhelming number of cases those employers are managed care organizations whose policies are generally inimical to quality psychiatric care. It is also apparent from the vote and the election patterns within the APA, that there is not a lot of political activism or interest for that matter. Hardly the behavior of a monolith.
The real difference with monoliths is the anonymity and secrecy issue. Every practicing psychiatrist is on record as being responsible to his or her patients. That responsibility is documented in medical records and pharmacy records. In any state, any physician can be reported to a medical board for practically any reason. Psychiatrists are held to the same professional standards as all physicians and that is a high bar, but it illustrates again - no monolith. I can beat my head against the wall all day trying to get a prescription authorized, but any complaint about me gets immediate attention and immediate scrutiny of my practice by the state medical board that I practice in, my employer, various committees or other state agencies, and in some cases my malpractice insurance carrier.
All of these factors combine to lead to more diverse interests and opinions that in any other field of medicine. As far as critics of the field, some of the best criticism comes from within psychiatry than from anywhere else. That does not prevent the various antipsychiatry factions from posting blanket criticisms of "psychiatry" (whatever that might be) and coupling it with any irrational or rhetorical criticism that they might like. I criticized some of this in the past and avoided most of the expected endless argumentation in response to my replies to these points. To me the rebuttals are factually no big deal, but critics of the monolith are so certain about themselves that they really don't do well with criticism directed back at them. I thought I would illustrate my point about monolithic psychiatry with some direct quotes from Robert Whitaker's book Mad in America. The page numbers are included for reference, but they are all from Chapter 7.
As recorded history would have it, things have changed and they continue to change. Psychiatrists can treat mental illness successfully across a number of settings and with a number of methods. It happens on a daily basis and it happens hundreds of thousands of times per day. It doesn't happen because monolithic psychiatry has a monopoly on the treatment of mental illness or a diagnostic manual. There are many more primary care physicians and non-psychiatric mental health providers (see supplementary 2). It happens because the treatment is successful and psychiatrists generally provide patients with the treatment and information that they need.
That is hardly the behavior of a monolith.
George Dawson, MD, DFAPA
References:
Robert Whitaker. Mad In America. Basic Books, New York, 2002. pp. 161-193.
Supplementary 1: The graphic at the top is from Shutterstock.
Supplementary 2: Psychiatry is dwarfed by the number of other mental health providers including 88,000 Family Practice specialists, 162,400 Internists, 100,000 psychologists and 120,000 Social Workers. I don't know the number of Psychiatric Nurse Practitioners or Physician Assistants whose primary role is to prescribe psychotropic drugs, but I will happy to add it if somebody has that information. Although I am sure that some of the physicians in these primary care groups don't prescribe some psychotropics, I am sure that 80% of all psychotropic medications in the US and most western countries are not prescribed by psychiatrists. So remind me again, what would Big Pharma get out of controlling monolithic psychiatry with pizza, donuts, and KOLs?
Thursday, June 4, 2015
Information versus Wisdom
I saw this post on another blog today and thought it was a good title. I end up pondering this idea almost every day. In medicine these days we are inundated by data scientists on the one hand and administrators on the other. The data scientists tell us how they are going to revolutionize medicine through their analysis of large data sets. The theory is that there are patterns in the data that can be detected only with advanced computational methods. Having gone through the spreadsheet era and seen how easy it is to prove almost any theory with a large spreadsheet, I am very skeptical of Big Data. Just dredging through the data, looking for patterns and writing it up does not seem very rigorous to me. It strikes me more like one of the popular TV shows where the agents are in the field but solidly connected to the computer whiz back at headquarters who is capable of pulling up any document, any floor plan, and hacking into any closed circuit TV system in order to get the information that is needed. I don't think that science works that way.
On the administrative side, it is the worst of times. The statistical efforts of administrators are frequently laughable attempts to legitimize the next genius idea to come down the pike. Their mistakes in healthcare are legendary ranging from the promise of the electronic health record to the RVU based management of physicians as widget producers, all exhaustively documented with numbers. I sat in a meeting one day that showed 95% of the physicians in the department were not "producing" enough to cover their salary. The problem was that nobody had done the multiplication on "work RVUs". When the appropriate multiplier was added it was a different story. Administrators also tend to collect a lot of numbers that they think will be useful for an analysis, without thinking ahead to the data analysis and statistics. They seem to have no idea about basic statistical analysis much less more advanced analysis like how to legitimately analyze data over time to detect real differences. There is no better example than the state of Minnesota collecting PHQ-9 scores over time from anyone trying to treat depression in the state. They seem to think that unconnected collections of those numbers at different points in time will have some kind of meaning. Administrators also have the habit of creating studies that confirm their vision of the world and when those studies are complete - that is all of the "proof" that is necessary. The entire concept of managed care rests on many of those studies.
On the wisdom side of things I can think of no better example than a colleague who I said goodbye to today. He worked with me for the past 2 1/2 years. He is an Internist who is also an Addictionologist and is ABAM (American Board of Addiction Medicine) certified. He has been a physician since the early days of the HIV/AIDS epidemic and treating those patients was a significant part of his early practice. He has an encyclopedic knowledge of the care of those patients and how it has evolved as well as being an excellent Internist. He is interested in psychiatry and can talk in psychoanalytic terms. He is also an expert in LGBT issues and can speak with authority on that subject. I certainly did not want to see him go, but for the purposes of this post, I can think of no better example of wisdom that comes with medical practice. He could be consulted on any number of complex problems in his areas of expertise and provide a very well thought out answer based not so much on information, but on what works and what the potential complications are. Any physician can tell you that these are the folks you want to work with. When I think about data mining approaches toward these areas of knowledge, I think about the 31 page document that is available online that looks at the issue of medication interactions of psychotropic and HIV medications. It is a compulsively great document, but lacks the wisdom to help you pick the best therapy for a manic patient on tenofovir.
Granted my position is a thoroughly biased one. I make no apologies for wanting to work with physicians who have the greatest technical expertise and know how to apply it. I don't mean people who can recite facts or even algorithms. I mean the people who know all of that and can look at the patient with the most complicated medical situation and still come up with a plan of action and how that patient must be closely monitored. They also know when it is better to do nothing at all and that is a difficult skill to acquire. Practically everyone leaves medical school and residency with a strong treatment bias. You are taught to be "aggressive" and that most of the treatments that you do will do some good even if there is not cure. In clinical practice, that is far from the truth. In psychiatry for example, you have to recognize that there are certain biological predispositions, clinical patterns, boundaries, and personalities that are the warning signs of disaster with certain treatments.
When I first started in medicine in the 1980s, the wisdom based model was still the predominate model in most clinical settings. Now it is much less frequent and there are departments that are just looking for people to fill in the gaps. They don't necessarily want to retain you they just want to "keep the numbers up." They also don't want you spending a lot of time on complex cases, because the payment rates rapidly decline if you are not shuffling people in and out the door. When the administrators start recruiting bodies based on their revenue models and Hollywood accounting, I hope that I will always end up on the side with the wisdom, rather than a heap of useless information.
There is a lot of that going around these days.
George Dawson, MD, DFAPA
Supplementary 1: I was going to jam in a section to comment on emotional and moral reasoning in view of the expected backlash to the Rosenbaum articles in the NEJM, but decided to add it here instead. It would have strained the above essay. It has been an interesting (and fully expected) exercise in political rhetoric. Predictably the critical articles mischaracterize her position and ironically are at least as guilty of the fallacies that they accuse her of using. In one case, a new fallacy is pretty much invented. I think it is instructive to note that in these matters, logic goes out the window. There is no pathway to a sound judgment. It basically involves rallying the troops to see who can shout the loudest. My self proclaimed bias above is part of the reason I am firmly on her side (but will refrain from the shouting). For anyone who thinks like me, there is no convincing me that the appearance of conflict of interest is the same as actual conflict of interest. There is no convincing me that free pizza and donuts will cause me to blindly prescribe a medication - probably because I have not eaten Big Pharma food since the early 1990s. In fact, if I think of a more plausible thought experiment about how much cold hard cash it would take to pay me off to prescribe a drug, I can't come up with a figure but it would have to be absolutely stratospheric compared with the usual speaker fees that people are listed in the Sunshine Act database for. All of that is based on the fact that I work for a living and treat real patients. I am accountable to those patients. If a medication does not produce real results or it causes too many side effects (like my early experience with paroxetine) it is off the Dawson formulary and I don't prescribe it again.
This is of course like arguing with Democrats and Republicans. I know that some pro-appearance of COI=COI will strongly dislike my experience and the way my thoughts on this matter are anchored in the way I practice medicine. That is the nature of arguing about emotional and moral reasoning in what the Institute of Medicine (IOM) describes as an ethical vacuum. The recent editorials certainly don't prove a thing.
The usual focus of these debates also leaves out the big picture that many entire University departments (math, science, engineering) actively collaborate with industries and in many cases actively invite industry participation in order to advance those fields. The notion that physicians are not able to do that because they have a sacred trust to patients and would be somehow compromised remains implausible to me, particularly when nearly all of the major decisions that physicians make in this country have been seriously tampered with if not controlled by managed care companies and pharmaceutical benefit managers for nearly 30 years.
That is a massive conflict of interest that nobody talks about and it affects 80% of all of the healthcare in this country.
Supplementary 2: The graphic at the top of the post is from Shutterstock.
Monday, June 1, 2015
Neurotic Kids
I was watching the FX comedy program Louie (Season 5 Episode 5) and encountered one of the funniest scenes I have seen on television. Louie is a neurosis based comedy, but it is also a show that many people will not be comfortable with because of content that results in the MAL warning. In this episode Louie takes his 10 year old daughter in to see Dr. Bigelow played by Charles Grodin. I heard that Grodin came out of retirement to play this character largely because he was impressed with Louis CK's technical expertise in filming the program. We met him in an earlier season when he was trying to dispel Louie of the notion that he has done anything to get rid of his back pain and instead focuses on the philosophical predicament of the three-legged dog that he is walking. After an introduction to the state of that animal he asks Louie: "What is the only thing happier than a 3-legged dog?" I won't give away the lesson but you can find it on YouTube.
In this episode, Louie has brought his 10 yr old daughter Jane in to see Dr. Bigelow. There are some preliminaries about whether she had a rash on her arm for 2 days or 30 days that has since cleared. From there Jane goes on to consider: "Weird things in my head." She is feeling like "I am sweating on the inside of my face" and builds this description with several "and then" clauses until she comes to a fantastic conclusion. Dr. Bigelow looks at her and without skipping a beat gives her a response that I have both heard from physicians and takes care of the problem. It also immediately shifts the frame from: "Is there something unusual about the way that Jane thinks?" to this being a completely acceptable exchange between a 10 year old and an old family doctor. I am not going to disclose Dr. Bigelow's punch line for those who have not seen this episode and I encourage you to watch it. It is worth it for this one scene that is so artistic, with timing so great, and it is the best acting from a child actor that I have ever seen. It is incredibly funny. I laughed out loud when I saw it and still laugh when I think of it. Dr. Bigelow's comment is an example of the implicit message: "I am taking you seriously at the neurotic kid level and not commenting on your behavior like you are a little adult." It also caused me to reflect on my childhood as a neurotic kid.
Neurosis is an old word these days. To me it always meant conflicted either in reality or at some symbolic level. If therapists are involved, the conflicts end up being conceptualizations based on their theoretical models. No matter how you cut it, anxiety is the common affect and there is usually a lot of it focused around unrealistic patterns of worry. The child psychiatrists that I know dismiss many of the eccentric behaviors they hear about and are unconcerned about what a lot of parents seem very concerned about. I have not assessed or treated children in over 25 years. My work comes at the tail end of childhood neurosis. The 18 year olds in high school and college students who become suicidal after their first boyfriend or girlfriend breaks off the relationship. It has given me the opportunity to advise them why they are hurting and about life in general. They seem to understand that by the time they get to my age that those problems in life will not hit them nearly as hard. I reassure them that when that happens, meeting me will be a distant memory and I will probably be the only psychiatrist they will have ever met.
But it wasn't that long ago that I was a neurotic kid myself. I won't disclose the full breadth of what happened to me so bear that in mind when you read about some of these incidents. The first bad sign was that I have never really slept well. Sixty years later that is still a problem. I am a chronic insomniac. I also recall vivid nightmares as a kid, with frequent visits from a being I called a "Deathalow." The Deathalow would just walk into my room at night and look very scary. It was the kind of behavior you see in a lot of horror movies, so this is probably a common experience. My parents and everyone else were puzzled because nobody had ever heard of a Deathalow. But they finally caught a glimpse of the inner workings of my mind when I started pointing at Catholic nuns and screaming: "Deathalows." Some time later, I pieced together the fact that Deathalows were a composite of a very bad chalk drawing of my grandmother's face in a nun's habit.
Just a few years later I was sitting in our living room watching television and I saw what appeared to be a Sir Walter Raleigh like figure walking up behind my father and preparing to stab him with a dagger. I shouted out what was happening and my parents freaked out. My mother was a frequent caller to our family physician and his advice was clear: "Stick him in a tub of ice water." No visit to the ER to see the crisis team, just ice water. They did so immediately, and while I was there I watched the comedy/tragedy masks on the walls in the bathroom laughing and crying while snakes slithered up toward the ceiling. That was at least until I cooled off. Then all of the hallucinations vanished. But it was the death of a family member that was all I needed to develop the longest preoccupation that I had in childhood - death and physical illnesses. For a while I was preoccupied with having cancer, rabies or being poisoned. I recall one incident after a Soviet nuclear test when we were warned about a large cloud of fallout passing over northern Wisconsin. We were advised to stay indoors. At the peak of that fallout, I can recall seeing radioactive particles floating in the air. The rabies preoccupation was the longest. I played football almost every day and was always alert to the presence of dogs. At one point, I thought that a dog may have had rabies and I had inoculated myself with the virus after I fell catching a pass. For months, I monitored myself for the development of symptoms of rabies. I would get up several times a night to look in the mirror to see if my physical appearance was changing (I was up anyway).
Around this time, I started to get nightmares about a large glass pyramid. There were several tiers of panels in the pyramid and on each panel was the face of a woman wearing Kabuki make-up shouting in a shrill voice: "Chinese ghosts!". In each case, I would wake up extremely anxious and wonder why I was dreaming that dream. And then... one night I decided that I really did not have to walk into that pyramid. It had a very long entrance-way. I thought before I fell asleep that night: "Just wake up if it looks like you are going into the pyramid, You don't have to go into that pyramid." And I was right. I woke myself up before the entrance to the pyramid and it was gone. I never dreamed that dream again. But the neurotic behavior in the daytime was harder to get a handle on for a long time. I had to tell myself that I had no control over if I lived or died. In some cases, I got some very negative feedback on the poisoning hypothesis as in: "Are you accusing me of poisoning you?" I eventually forced myself to think of other things. Eventually that forced aspect was gone as I developed more interests. As my reading and research in other areas increased, my worries about cancer, rabies, and death dissipated.
Throughout all of this, I never saw a counselor, therapist, or psychiatrist. I got the "Dr. Bigelow advice" from our family physician with treatments ranging from "throw him in a tub of ice water" to a rather primitive creosote-like nasal lavage that all of the kids in my family got if we went in to see him for a cold. I am convinced it was an aversive therapy to keep us out of his office. I have never seen that treatment used anywhere else in medicine.
This merely scratches the surface of my experience as a neurotic kid. It may be why I got such a laugh out of Dr. Bigelow's advice. And of course it also causes me to wonder what would have happened if I had received psychotherapy or medication for these "symptoms." Would I have encountered one of the wise child psychiatrists I know or somebody who thought I was psychotic? I was definitely not as calm about it back then as I am recalling it now - there were after all snakes on the walls!
But I eventually turned it around on my own and became a guy who can appreciate the humor in being a neurotic kid and somebody who can relate to them.
George Dawson, MD, DFAPA
Supplementary 1: No guarantees on how you will find Louie. I find much of his comedy brilliant, but some is also cringeworthy so as always watch at your own risk. The segment I am talking about is less than 2 minutes long about 2 1/2 minutes into Season 5 Episode 5.
Supplementary 2: To all my psychiatric colleagues out there, I did think about these disclosures. Hardly anybody reads this blog and I don't anticipate doing any transference based psychotherapy. I think it is also pretty obvious that you reach a point in your life where all of these neurotic behaviors are irrelevant. All of the other main players are dead or forgotten and there is no emotional impact. The experiences themselves are history and have been for 50 years. That is how I chose the disclosures. In part they were also modeled on some disclosures I have read in books written by psychiatrists who disclosed things that happened to them as adults.
Supplementary 3: The more I reflected on the historical context of neurosis, the more I realized that it means something different now than when I was a kid. When I was a kid, it meant that you were crazy in the popular sense of the word. Nobody had a nuanced appreciation of mental illness and how anxiety or obsessions were different from psychotic disorders. Today, I think neurotic behavior is reinforced to a point. For example, the parents who say: "He or she is 12 going on 30" and seem to see their children as small adults who may need some competitive advantage like cognitive enhancement.
Supplementary 4: The glass pyramid graphic is a download from Shutterstock for non-commercial use only and this is a non-commercial blog.
Supplementary 5: A useful interview question for adults with anxiety and depression: "There are all kinds of theories about how people get anxious. One of those theories is that our minds come up with stories to fit the level of anxiety that we have. That can be transmitted from one person to another. Looking back on your childhood can you recall anyone who seemed to transmit their anxiety to you?
Sunday, May 31, 2015
The NIMH Director and the RDoC - The Politics and The Science
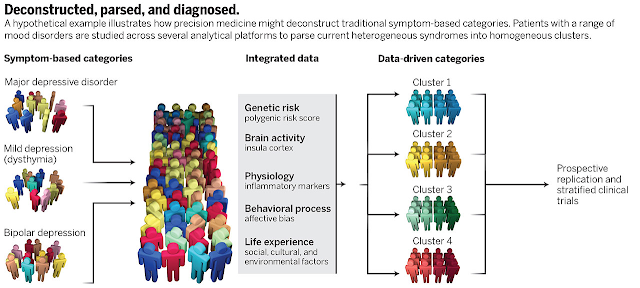 |
from: Insel TR, Cuthbert BN. Medicine. Brain disorders? Precisely.
Science. 2015 May1;348(6234):499-500.
|
I caught this article about the RDoC criteria for classifying mental illnesses based on various non descriptive parameters and neuroscience in the journal Science a couple of weeks ago. As any reader of this blog can attest, there is no stronger advocate for the role of neuroscience in current psychiatric practice and the future of psychiatry than me. There has been media controversy on this subject and it is always difficult to determine how much real controversy exists and how much of it is just made up for the sake of media self promotion like much of the DSM-5 controversy was. Reading through the article by Thomas Insel and Bruce Cuthbert there are statements that can be taken at face value. I think these statements are consistent with the position that clinicians in general are not very scientific and are also outright clueless in some areas. This is a bias that I have certainly heard from other scientists and it does not serve the cause of science very well, especially if the goal is to advance neuroscience and bring everyone up to speed on that discipline. Dr. Insel has presented his view that all of the trainees in the clinical neurosciences of psychiatry, neurology, and neurosurgery should rotate through a year or two of a shared neuroscience. When I first heard him present it five years ago I thought it was a great idea. In the time since and especially after getting a response from him, I think it is less clear. It would be great if every department of psychiatry had neuroscientists on staff to teach neuroscience. But they don't and there is also the problem of neuroscientists being focused on research rather than teaching. On the other hand, there are plenty of bright people in those departments who know a lot about the brain. It is a question of reconciling these two points to come up with the necessary infrastructure yet in this article the authors make it seem as if large clinical problems are not addressed and that clinicians are fumbling around with very crude assessment methods.
They list three articles as examples of the RDoC. The most interesting of these articles is one from the American Journal of Psychiatry that proposes that computer abstracted data from hospital notes that is converted to RDoC criteria are better predictors of hospital length of stay (LOS) than DSM criteria. Just considering that method my first impression was that there was a lot wrong with that picture. First of all, LOS data is tremendously skewed based on non-clinical practices. All it takes is hospital case managers with some success in intimidating physicians to skew the data in favor of business rather than actual medical or psychiatric discharge decisions. Second, the quality of data from inpatient settings is incredibly bad due to the toxic combination of electronic health records and government billing and coding regulations. As a reviewer, I have seen thousands of inpatient records, some of them hundreds of pages in length and I have found EHR records are notoriously poor in information content. And finally, I thought the RDoC was a new system designed to be dependent more on neuroscience than the DSM-5? How does methodology that looks at this DSM biased, sketchy clinical data result in a RDoC diagnosis? Looking at the graphic from the Science article at the top of this post, it is pretty clear that 3 out 5 data dimensions under "Integrated Data" are basically clinical data. There is a smugness displayed in the report similar to what might be seen in a rant by an antipsychiatrist: "For now clinicians might be best advised simply to be aware of the usefulness of dimensional models to capture psychopathology." and "This result should provide some reassurance to clinicians that their notes do contain relevant detail for deriving dimensional measures of illness; like Molière’s Bourgeois Gentlemen speaking prose without knowing it, clinicians may already speak some RDoC."
Really?
The average person I see has chronic insomnia and has had possible sleep terrors and nightmares in childhood along with social phobia. At some point they developed either severe anxiety or depression, but they can't recall the sequence of events and they currently have both. They typically think that they have had "manic episodes" and may have been diagnosed with bipolar disorder even though they don't know what a manic episode is. All they know is that their symptoms have persisted usually without remission for the past 10 to 15 years. Of course that is complicated by the fact that they have been using marijuana, alcohol, and opioids in excessive amounts since then, they may not have a significant family history of psychiatric and addiction problems, and they have the expected childhood adversity and adult markers of psychological trauma and abuse. Further, I know from talking to the same people in repeated initial evaluations over the years that they don't give the same history twice and rarely remember much about their medications or psychotherapy treatment. Should I use a "placeholder diagnosis" (pejorative term from reference 4) or should I assume that I am dealing with the social phobia that the patient may have had in childhood? The idea that an RDoC diagnosis is going to give me an answer to that question any better than a DSM-5 diagnosis is pure folly if you ask me. At least until we get the promised neuroscientific markers promised by the NIMH. In fact, the description of the RDoC in these articles is reminiscent of another technology that was supposed to diagnose mental illness and that was quantitative EEG or QEEG. I know quite a lot about QEEG, because I purchased a machine in the 1980s after a promising article on the technology came out in the journal Science. I researched it using highly skilled EEG techs and an expert in neurophysiology to run the protocols, and concluded the diagnoses that came from the computerized analysis of the tracing were no better than chance in terms of what patients presented with. Like RDoC diagnoses, the computerized analysis of QEEG data was highly dependent on the input of clinical data collected by the clinician. It allowed the clinician to add and subtract clinical variables and look at how the diagnosis varied.
The staff and researchers at the NIMH need to decide if a superior and critical attitude toward physicians who use current clinical approaches and are successful with them is the best one. It should be obvious from the above analysis that many of us are not as naive or as ignorant about science as they expect. My proposed solution would be a more collaborative approach including the following:
1. Recruit and train neuroscience teachers - most of them are already out there. For example much of what I teach to trainees interested in addiction and addiction medicine is neuroscience. It is also much more realistic than waiting for every department to have access to neuroscience researchers and then expecting those researchers to teach in addition to doing research. My guess is that every Psychiatry department already has faculty that teach neuroanatomy, pharmacology, brain science and neuroscience already and that most of them are not officially scientists.
2. Make the reading list available online - the article refers to over 1,000 published articles that focus on the RDoC criteria. These should be available though the National Library of Medicine web site along with other neuroscience articles of interest to psychiatrists. An added bonus would be CME activity available for self study.
3. Post a list of neuroscience modules and build on that list - In a previous post, I posted two links to neuroscience modules through the NIMH. I would put up two lists, one containing a growing list of modules and the second with a list of the neuroscience concepts that need to be illustrated. This would be useful for psychiatrists, psychiatrists in training, and medical school professors hoping to make their basic science lectures more relevant, since many clinicians still seem to have difficulty understanding how neuroscience is important in psychiatry.
4. Better graphics - make high resolution graphs that illustrate detailed brain anatomy and basic science available online for teachers. Pulling this material together is often the most difficult part of the teaching job and it requires an intensive effort to not run afoul of copyright laws. It would be easier to recruit neuroscience teachers if there are high quality teaching materials available.
5. A neuroscience teaching blog - In addition to the NIMH staff posting the references, concepts and modules, an open teaching blog should also be available. I would encourage it to be a platform for discussing concepts and how to present them to trainees. Ideally, it would be a place for active dialogue about the concepts and teaching them.
I think that all of these measures would be helpful in building an infrastructure of neuroscience teachers, neuroscience teaching, and a mechanism for the widespread dissemination of this material in residency programs and in educational programs for practicing psychiatrists. If the RDoC is in fact worthwhile, there is plenty of brainpower outside of the NIMH to figure that out.
It is the brainpower that is currently focused on coming up with solutions and resolving problems of incredible clinical complexity. And that happens every day.
I plan to send these recommendation to Director Insel and see what he thinks.
George Dawson, MD, DFAPA
1: Insel TR, Cuthbert BN. Medicine. Brain disorders? Precisely. Science. 2015 May
1;348(6234):499-500. doi: 10.1126/science.aab2358. PubMed PMID: 25931539.
2: Casey BJ, Craddock N, Cuthbert BN, Hyman SE, Lee FS, Ressler KJ. DSM-5 and RDoC: progress in psychiatry research? Nat Rev Neurosci. 2013 Nov;14(11):810-4. doi: 10.1038/nrn3621. Review. PubMed PMID: 24135697.
3: NIMH. Research Domain Criteria
4: McCoy TH, Castro VM, Rosenfield HR, Cagan A, Kohane IS, Perlis RH. A clinical perspective on the relevance of research domain criteria in electronic health records. Am J Psychiatry. 2015 Apr;172(4):316-20. doi: 10.1176/appi.ajp.2014.14091177. PubMed PMID: 25827030.
2: Casey BJ, Craddock N, Cuthbert BN, Hyman SE, Lee FS, Ressler KJ. DSM-5 and RDoC: progress in psychiatry research? Nat Rev Neurosci. 2013 Nov;14(11):810-4. doi: 10.1038/nrn3621. Review. PubMed PMID: 24135697.
3: NIMH. Research Domain Criteria
4: McCoy TH, Castro VM, Rosenfield HR, Cagan A, Kohane IS, Perlis RH. A clinical perspective on the relevance of research domain criteria in electronic health records. Am J Psychiatry. 2015 Apr;172(4):316-20. doi: 10.1176/appi.ajp.2014.14091177. PubMed PMID: 25827030.
Supplementary 1:
The above figure is licensed through the American Association for the Advancement of Science - license number 3637270124183.
Friday, May 29, 2015
Minnesota Finally Rejects Managed Care
In a rather stunning reversal of thirty years of public policy, the Minnesota Legislature voted last week to fund for a "network of small treatment centers" to compensate for all of those years of rationing. The details are still vague but it is described in the StarTribune article by Serres as a "network of small treatment centers, to be built across the state, anchoring a broad package of preventive services so children don't end up in emergency rooms or inpatient psychiatric wards where many of them are discharged prematurely for a lack of beds." The funding is about $13 million for 2 years and $6.6 million "to create a network of 30-bed treatment centers for children with highly aggressive or self-injurious behaviors, who are often turned away from hospital inpatient units." Political speak is evident in that sentence. I can't imagine that $6.6 million or even $19.6 million gets you a lot of 30-bed treatment centers. Later in the article a total new bed capacity is described as 150.
The author of the article is oblivious to how this all happened in the first place. Was Minnesota an idyllic place with no mental illness in the first place? Did the problem arise because an epidemic of mental illness? Absolutely not. Thirty years ago, the state had more bed capacity and more treatment options for both children and adults with mental illness. Minnesota is a state with massive managed care presence and those managed care companies currently run all of the acute care psychiatric beds in the state - for both children and adults. Once managed care companies learned that they could deny hospitalizations based on some fictional "dangerousness" criterion and otherwise ration psychiatric services at multiple levels there was - in effect - no rational psychiatric care. As I have posted on this blog many times, people are discharged from hospitals in a few days essentially without treatment, treatment units are chaotic without a therapeutic environment, people who require medical detoxification form drugs and alcohol are generally out of luck, and it creates and ongoing demand on emergency departments and correctional facilities. All it took was getting these practices embedded in the state statutes and setting up a cursory review of complaints against managed care companies at the state level to seal the deal. The reporter in this case makes it seem like the Minnesota Legislature and a "bipartisan coalition of lawmakers" are solving a problem. This is a problem they created in the first place and I will believe in a solution when I see it.
I have some first hand knowledge of the problem with children's services from my contact with child psychiatrists around the state. Their experiences are echoed in the story in this article of what happens when your child is out of control and nobody is willing to help. The family in this case describes a 17 year old boy with severe mood problems, aggressive thoughts and thoughts of self harm. He was hospitalized 6 times and discharged in a heavily medicated state. He was turned down by 30 residential facilities before being accepted by an out of state facility. His parents describe themselves in a "perpetual state of anxiety" trying to manage all of these scenarios. But the most incredible line in the article:
"For years, children who exhibit highly aggressive or violent behavior in Minnesota have been forced to drift from one short term hospital to the next, often returning to their families heavily medicated but with their illnesses largely untreated."
This is not surprising to any psychiatrist. This is the end product of managed care rationing and it occurs whether the patient is a child or an adult. It happens when businesses and governments collude in providing some bastardized version of psychiatric care. It happens when psychiatrists in this case are ignored. When state officials ignore psychiatrists. When psychiatrists who are trained to treat aggressive and violent behaviors are not allowed to do their jobs. After all, why would anyone with aggressive behavior because of a mental illness be turned away from a psychiatric unit? Aggressive and suicidal behavior are the main reasons that psychiatrists exist today. It is what we do. Let us do our jobs.
So far this is one small victory for children's mental health advocates and my cap is tipped to them. But to reverse more of the problem we need to acknowledge what it is and it is managed care or more specifically their marketing word for mental illness - behavioral health.
Let's get rid of it entirely.
George Dawson, MD, DFAPA
Reference:
Chris Serres. Facing chronic shortages, Minnesota's mental health system gets a boost. Minneapolis Star Tribune, May 29.
Supplementary 1: The image used for this post is of Dexter Asylum attributed to Lawrence E. Tilley [Public domain], via Wikimedia Commons. The original image was Photoshopped with a graphic pen filter.
Supplementary 2: For a detailed post on some of what happened try this.
Sunday, May 24, 2015
Physicians Replaced By Computers - Lessons From A Roomba
My Memorial Day project was purchasing a Roomba and getting it up and running. I am a big believer that robots will make all of our lives easier at some point and decided now is the time to start walking the walk. For those not familiar with the Roomba, it is designed as a robotic vacuum cleaner. Once you have set up the rooms and programmed it, it is basically supposed to vacuum your floors automatically and then park itself in a docking station for charging. The machine itself is about a 14 inch diameter disk that rises to a height of about 3 1/2 inches off the floor. It is a light 8.4 pounds. It is able to accommodate sharp angles with a secondary brush that spins on an arm that extends from under the main disk. This combination of the main disk spinning and the extended spinning brush cleans the corners of a room. I purchased the latest model, a Roomba 880 after consulting with friends and relatives who had earlier models.
One of the considerations in buying the Roomba was whether it would help turn my home into an even cleaner environment than it currently is. That is a tough act. One of my friends who is a physician gave his opinion that my home is "museum-like". My office is probably the only problematic room with stacks of books and journals piled everywhere. Disarray certainly but minimal dust. My entire first level is hardwood flooring that is typically vacuumed with a built in system. To its credit the Roomba contains all of the debris in the machine until it is emptied and all of the exhausted air is HEPA filtered to avoid exhausting any dust particles. The main cleaning mechanism consists of two debris extractors that are rubberized bars that spin at a high rate of speed across the floor surface to capture dust, hair and larger particles. But the most interesting aspect of the Roomba was going to be its observed behavior. It has two modes when vacuuming. It can start in a spot and spin increasing circles in an outward direction until gets to about a 3 foot diameter and then it spirals back in to the center spot. In the more typical mode it heads to the room perimeter and then "automatically calculates the room size and cleaning time." The most valuable tip in the manual was to take measures to restrict it to one room at a time and it comes with two Virtual Wall®LighthouseTM devices that allow for easy demarcation of the work area.
The most fascinating aspect of getting started with the Roomba was going to be setting it up and watching how it went about the task of vacuuming. I did some very minor room preparation, charged it up, and turned it loose. As expected it headed straight for a wall and then attempted to establish the perimeter. I remembered this as standard rodent behavior. If you have ever confronted a mouse in an open area of your floor, their first move is to dash to the baseboards and run parallel to them to escape. That strategy works well in the wild because the maneuver is associated with more cover and makes them less susceptible to predators. It works much less well when confronted by a human who knows that it is their first move. And yes, scientists have bred mice that do not exhibit this behavior. My guess is that they would not fare well if they made it outside the lab. The Roomba's behavior is less rigid than a typical mouse with some exceptions. In the hour and 20 minutes it took to vacuum the adjacent kitchen and great room - it circled a kitchen island perfectly at least 10 times, but at the wall perimeters it was much less predictable. At times the Roomba would peel off and take off across the room in a single pass or rarely return and continue along the original wall. Sometimes it would head off the wall at a 45 degree angle and at other times 90 degrees. There were never the usual adjacent passes that a human would make using a standard vacuum cleaner.
According to the literature, the Roomba is supposed to "crisscross" the room in order to clean the floor. I placed two small pieces of popcorn in the middle of a large section for flooring to use as markers of cleaning efficiency. In the course of an hour, the Roomba passed these markers many times, sometimes very closely without vacuuming them up. During that time it was very difficult to detect how much crisscrossing had occurred since mouse-like it spent the majority of the time in the periphery, bumping and spinning around walls and furniture. It eventually did break free from the walls and set off on a 45 degree path picking up one popcorn fragment at about the one hour mark and the other at about one hour and ten minutes. The old adage about pictures is true and I happened across this 30 minute time lapse photo of the Roomba working a room (with permission from the SIGNALTHEORIST web site). It correlates well with my description of the actual paths.
As I surveyed the job afterwards, the floor was definitely clean and the warning light on the machine was saying that the dustbin was full. When emptied, it contained an impressive amount of debris and dust relative to what seemed visible to the naked eye. Another win for the robots? Well, not really. It is an interesting tool that I will continue to use and study, but in comparison with humans it is not efficient and at this point certainly not autonomous. Despite all of the guidance in the manual the Roomba can still encounter unpredictable surfaces and get itself into trouble. In my case it was the pedestal of a recliner. The wood at the edge was about 3/4 of an inch high. For some reason, the machine did not recognize it as an obstacle and continued to run up the base and get hung up. A loud spoken error message would sound advising the human in the room to pick it up and start it in a new place. The other concern is efficiency. It spent far too much time in the perimeter and a low percentage of time covering the main floor areas. That was tremendously inefficient. It took at least 5 times longer to vacuum the main rooms than I would have if I was pushing a vacuum cleaner. Even though it allows me to do other things, it says something about current state of available and affordable domestic robots. They can't match the performance of humans on a fairly basic task. This is an important concept.
Before any of the futurists out there jump on me for being a Luddite, let me disclose a few details. I am a member of the IEEE and have been for the past 18 years. I am currently a member of the IEEE Robotics and Automation Society. I am not an electrical engineer and I have not designed or built any robots, but hope to start doing this when I retire from psychiatry. I consider myself to be an expert in the human brain and the advantages it confers on humans over other animals and machines. The Roomba is a basic case in point. It cannot sense and adapt to novel conditions quickly enough to match a human doing the same task. Even more striking is that although it is designed to vacuum homes and I have a fairly typical home with a better than average floor surface, it still encounters situations that exceed its response capacity. In those situations it needs a human assist. What is it about the human brain that leads to that kind of an advantage? First and foremost, it is a rate of pattern matching and pattern completion capacity that allows us to recognize vacuuming problems, anticipate them and correct them by developing novel solutions even before the problem leads to a stop in action. Some of this happens when a human goes around the room to set it up for the first time for the Roomba. That human has made some assessment of the machines capacities and limitations and is problem solving for the machine before it is turned on.
Observing the limitation of the Roomba leads me to a point where I can address both the idea of computers replacing doctors and how that fits into the common anti-physician narrative in this country. Is there a connection between the two? My experience tells me that there is. For nearly 30 years there has been a constant stream of antiphysician rhetoric. The sources have been expected. One of them is the key opinion leaders (KOLs) of the managed care industry. I can recall reading one of the the first books written by one of them, a non-physician who was widely acclaimed as being an expert in managed care. His early theory was that the high cost of health care was due to the decisions that physicians make. But in the middle of the book he wrote what he thought of physician salaries and only grudgingly acknowledged that they should probably be paid a good wage due to their education. I have posted here many times my experience at a managed care conference in the 1990s. The speakers at that conference were very clear that the explicit agenda of their industry was to replace all of the specialists with primary care physicians. The examples given were orthopedic surgeons and psychiatrists. When a psychiatrist in the crowd pointed out the shortcomings of that philosophy - he was called a "whiner" by a Governor who was an anointed KOL in the industry. Then the KOLs from the financial services industry started weighing in. You could find glimpses of it while reading the investment literature. People who were investors with no particular degree started saying that some day, physicians would get what they deserve - with the implication being that whatever that was - it was not good. Any physician has experienced this prejudice. The comments about how physicians are "expensive" as a rationalization for working them to death by not hiring any additional help. Replacing physicians with computers seems like a logical extension of this rhetoric. Googling this topic returns a number of provocative articles written from a point of view that is generally consistent with who the author is.
I know that some of those authors know the difference between a robot or a computer and a doctor, but it is also clear that some do not. They certainly don't seem to understand that the real processing power of a human diagnostician's brain is in the area of pattern matching. In order to duplicate that property with current technology, takes a massive computer and it is one of the reasons why my new $700 Roomba, although well designed - can easily be beaten by a human with a standard vacuum cleaner. But the human advantage goes far beyond that. Human diagnosticians do far more than match simple patterns. They are able to complete fragments of patterns and anticipate what the whole pattern should be. For example, is it likely that a depressed person is in this current state as the result of an inherited form of depression, their current state of detox from an opioid and/or benzodiazepine, current stressors or interpersonal conflicts, brain trauma, an undiagnosed medical condition, childhood adversity, psychological trauma as an adult, or defects in reasoning at either the emotional or cognitive levels. Then there is the matter of acquiring all of the data to make the determinations. Patterns upon patterns of data. The Roomba-like approach would be to give the person a checklist of depressive symptoms and pretend that is all that needs to be known. Checklists are already being administered by a computer and may be administered by robots someday.
Yet it takes the pattern recognition, and several layers of it, as well as human experience dependent learning in order to make a real medical or psychiatric diagnosis.
George Dawson, MD, DFAPA
Supplementary 1: The graphic at the top of this post is a photo that I shot of the inside of the box that my Roomba came in.
Supplementary 2: I don't want to give the false impression that I do a lot of vacuuming. My wife does practically all of it, but I am trying to do more especially if there is a high tech twist to it. Some of the first robotics I hope to work on will be human controlled arms and hands designed to do yard work and move heavy objects around in the house. I can't believe this is an area that has been ignored.
Subscribe to:
Posts (Atom)