The New York Times somehow let an all
too true story about the treatment of mental illness slip through today instead
of one of their more typical speculative pieces. It is a story of a
family desperately trying to get their father and husband assistance after he
develops acute bipolar disorder with psychotic symptoms. It is
a reasonable discussion of some of the issues behind deinstitutionalization,
involuntary treatment, and the sad state of affairs
that currently exists in trying to get treatment for those with
severe mental illness.
Probably the best quote in the article follows:
“The lack of resources has triggered a devolution of the
standard,” says Robert Davison, executive director of the Mental Health
Association of Essex County, a nonprofit group that connects patients to
services in northern New Jersey. “Twenty years ago, ‘imminent danger’ meant
what most people think it means. But now there’s this systemic push to divert
people away from inpatient care, no matter how sick they are, because we know
there’s no place to send them.”
I will refrain from the typical term applied to the situations
whose definition is: "a particularly bad or critical state of affairs,
arising from a number of negative or unpredictable factors". The reason I will refrain is that it is not exactly accurate.
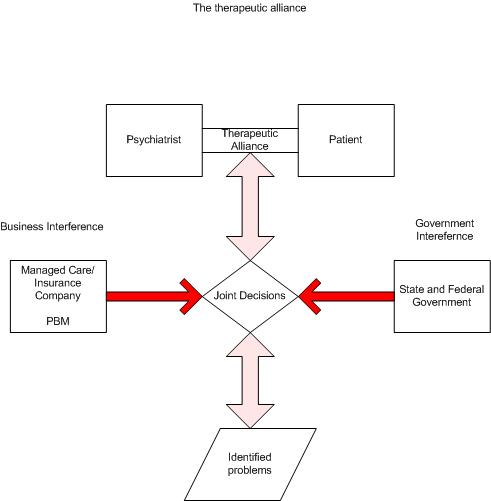
The entire debacle has been totally predictable. It is the predictable
result of applying managed care rationing techniques to the private and public
mental health sector and denying care to those people with the most severe
forms of mental illness. When your only perspective is rationing care to make money - there are no standards.
So what are the solutions?
They are fairly straightforward. First off, there
needs to be reasonable commitment standards with a more appropriate balance
than "imminent dangerousnessness". From the article it is clear
that even that standard is interpreted widely. There needs to be a three
part standard for danger to self, danger to others, and gravely disabled and
not able to care for oneself. Some states accomplish the same goals by
separating civil commitment from protective
services/protective placement statutes. The latter approach has
the advantage of avoiding the use of commitment courts for issues that come up
in the course of Alzheimer's disease and other dementias.
Secondly, the statutes need to be
uniformly interpreted. My experience working with probate courts
from a 3 county area illustrates that no two judges would make the same
decision on a particular case. In many counties, the social workers
screening the cases had much different philosophies. The only time that
changed was when there was a bad outcome. That outcome was typically a
person released by the court who attempted or committed a homicide or suicide.
Third, there needs to be recognition that
state hospital beds are not the only solution. The main reason
that state hospital beds don't work is that there are no local resources.
Once a person is ready for discharge, there is no place to send them.
More and more people accumulate at the state hospital and nobody is
discharged. There needs to be housing resources and community teams to actively
work with people to facilitate discharge and maintain them in the
community. Just building state hospital beds has the
predictable outcome of building more state hospital beds.
Fourth,
financial conflicts of interest must be eliminated. They exist
at multiple levels and are the predictable outcome of rationing techniques that
originated in the managed care industry 30 years ago. The basic premise
of managed care is that a "medical necessity" standard can be
developed that will be subjectively interpreted by the company in order to
ration care and save the company money. One of the major loopholes has
been any person that needs involuntary treatment. The managed care
company can simply say this care is no longer "acute" or
"medically necessary" and transfer the financial burden of care
to the taxpayers. Huge cost savings to the managed care company.
That doesn't happen if you need a heart transplant.
The financial conflicts of interest
occur at every level in the system. Another example is the interpretation that at an aggressive or
self endangering event has to have occurred in order to meet the
commitment standard. The author here does a good job
of providing examples. What is not obvious is the financial
conflict of interest that is present in these situations. In almost all
cases - the hearing occurs at the county level and the judge presiding
knows the county's financial status and access to resources. That
significantly biases decisions especially in the case of counties where there
are limited resources.
The only solution to avoiding these
pure conflicts of interest is to have the money follow the patient and
have it in a dedicated fund. It is too easy to move funds around that
should be designated for the treatment of severe mental illness if they move in
and out of a general fund.
Fifth, there need to be better
managers of the systems responsible for the care of patients with severe mental
illnesses. Managed care companies clearly do a very poor job.
On the other hand every state generally has a large Department of Human
Services and second to education they are usually the largest budget in the
state. Despite significant constant and high demands they are
generally managed like any other state agency. If there is a
revenue shortfall and everybody has a 6% across the board spending cut, DHS
also has a 6% spending cut. These departments usually employ cost
center accounting that is also a detriment to coming up with
an adequate plan of care across treatment settings. Finally it
is also common these days in both managed care and state systems
to see managers with no clinical experience attempting to hold
clinicians accountable to subjective standards and
implementing plans to change care delivery -
even though they have no expertise.
These are a few changes that would
make a world of difference for families and patients like those mentioned in the NYTimes article today. I am not
very hopeful that they can happen because it would also involve changing a
culture that has been the most insidious aspect of managed care. That
culture is quite simply - bureaucrats and business people telling psychiatrists
what to do and restricting the resources needed to provide adequate care.
George Dawson, MD, DFAPA
Jennen Interlandi. When My Crazy Father Actually Lost His
Mind. NYTimes
June 22, 2012.